REVIEW ARTICLE
Can Metastatic Colorectal Cancer Be Cured?
By David L. Bartlett, MD1,3, Edward Chu, MD2,3 |
March 13, 2012
1 Division of Surgical Oncology, Department of Surgery
2 Division of Hematology-Oncology, Department of Medicine and Pharmacology & Chemical Biology
3 Molecular Therapeutics Drug Discovery Research Program,
University of Pittsburgh Cancer Institute, University of Pittsburgh
School of Medicine, Pittsburgh, Pennsylvania
ABSTRACT: Significant advances have been made in the
treatment of metastatic colorectal cancer (mCRC). Development of the
targeted biologic agents and their integration with cytotoxic
chemotherapy regimens has led to improvements in clinical efficacy.
Despite these gains, the overall impact of these combination regimens in
mCRC therapy has been relatively modest. While 2-year survival has
improved, substantive gains have yet to be made in 5-year survival.
However, a small subset of patients can be cured of their metastatic
disease, with prolonged 5- and 10-year overall survival. This select
group of patients includes those with metastatic disease limited to the
liver or other organ-specific sites, as these patients are able to
undergo surgical resection at the time of diagnosis or following
conversion therapy with the appropriate integration of chemotherapy. A
multimodality team-based approach involving medical oncologists,
surgical oncologists, radiologists, and other healthcare providers is
absolutely critical for the success of this therapeutic approach. This
article reviews the main issues that must be considered from the
surgical oncology and medical oncology perspectives, respectively.
In
2012, colorectal cancer (CRC) continues to be a major public health
problem. In the United States this year, there will be an estimated
147,000 new cases diagnosed and nearly 50,000 deaths resulting from this
disease.[1] Worldwide, approximately 1 million new cases of CRC are
diagnosed each year, with nearly 500,000 deaths attributed to this
disease annually. About 25% of patients present with metastatic disease,
and of this group, 50% to 75% will have disease confined to the
liver.[2-4] In patients who present initially with early-stage disease,
up to 50% will eventually develop metastatic disease, with the liver
being the most common site. Another 10% to 20% of patients will present
with disease involving the lung and other less common sites of
metastatic involvement, including the peritoneum, ovaries, adrenal
glands, bone, and brain.[5,6]
When metastatic disease is limited to an
organ-specific site, an important consideration is whether the disease
is resectable at the time of initial diagnosis or whether it is
initially deemed to be unresectable but may become resectable with the
up-front use of chemotherapy. With the integration of chemotherapy and
surgical resection, overall 5-year survival rates on the order of 30% to
40% can now be achieved. A multidisciplinary, team-based approach
involving surgeons, medical oncologists, radiologists, and other
healthcare professionals is required to determine the optimal timing and
sequence of surgery and chemotherapy.
This article reviews the
multidisciplinary approach to patients who have organ-limited metastatic
CRC (mCRC), with the main focus being on liver- limited disease. In
particular, the surgical and chemotherapy aspects of disease management
will be discussed.
Historically,
the setting of liver-limited metastases from CRC has been one of the
few examples of curative metastasectomy in oncology. Even before the
development of effective chemotherapy agents, surgical resection of
limited hepatic metastases was associated with prolonged survival and
cures.[7] Several important prognostic factors, such as disease-free
interval, number and size of metastases, presence of extrahepatic
disease, and stage of the primary cancer, have all helped to define the
expected cure rate for hepatic metastasectomy. For patients with
metastases defined by the most favorable prognostic categories, cure
rates of 24% have been achieved with surgery alone.[8] The indications
for surgical metastasectomy were for patients with disease limited to
the liver, a total of four or fewer metastases, unilobar involvement,
tumors of less than 5 cm in their greatest diameter, and a disease-free
interval of at least 6 months.[9-12] It is, therefore, not surprising
that the development of more effective chemotherapy has led to a
significant improvement in overall survival and cure rates, as well as
an expansion of the indication for metastasectomy. This indication has
evolved into resection of any disease that allows for adequate hepatic
residual volume for liver regeneration and survival, assuming there has
been a response to neoadjuvant chemotherapy.[13] In the past, surgeons
were appropriately concerned that resection of visible disease would be
followed by rapid recurrence from microscopic metastases in the residual
liver. However, incorporation of effective neoadjuvant and/or
conversion chemotherapy, as will be discussed in this article, provides
greater confidence that micrometastatic disease can be eliminated and
that removal of gross disease can lead to long-term cure. In addition,
as hepatic surgery has become safer and easier for the patient, there is
now wider acceptance of incorporating hepatic resection into a
multimodality strategy to prolong survival.
The options for local
and regional treatment of hepatic metastases have become broad, and
include surgical resection, local ablation therapy, hepatic arterial
infusion therapy, transarterial chemoembolization, radiomicrosphere
therapy, and isolated hepatic perfusion.[14,15] Each of these approaches
has been associated with long-term cures, although surgical resection
and local ablation strategies have been the most effective. The goal for
surgical resection is to achieve a negative microscopic margin. Given
the concern about microscopic extension beyond the visible tumor, a 1-cm
margin around the tumor is ideal. Numerous coagulation devices exist to
enhance the safety of parenchymal transection by limiting blood loss.
Minimally invasive approaches, such as laparoscopic and robotic
assistance, have become commonplace, and they are associated with
reduced blood loss, shortened hospital stay, and decreased narcotic
usage postoperatively.[16,17] For patients undergoing multimodality
therapies, minimally invasive surgery may also improve quality of life
during treatment and decrease the recovery time necessary before
adjuvant chemotherapy is administered. The options for resection include
extended lobectomy, lobectomy, segmentectomies, and nonanatomic wedge
resections. Many surgeons remove the least amount of liver tissue
feasible to preserve the anatomy for future resections, if necessary,
while others prefer formal anatomic resections in order to provide the
best chance of a negative margin. These two approaches have not been
directly compared in a randomized trial; however, retrospective data
suggest that the ability to achieve a negative margin, as opposed to the
specific type of resection, determines long-term prognosis.[18]
Local
ablative approaches have provided an alternative to surgical resection
for patients with mCRC. These approaches include radiofrequency ablation
(RFA), microwave ablation, cryotherapy, and focused radiotherapy (eg,
using the CyberKnife). RFA is a reliable technique to ablate metastases
up to 5 cm in size. However, it has limited efficacy in centrally
located tumors in which proximity to the main portal triads or hepatic
veins may cause bile duct injury, extensive hepatic necrosis, or
inadequate tumor cell death adjacent to the vessels. The potential
advantages of these local strategies over surgical resection include
enhanced safety, outpatient percutaneous treatment options, and the
ability to preserve hepatic parenchyma. The local recurrence rate after
local ablative procedures is clearly higher than with surgical
resection, with rates as high as 34% having been reported.[19] The local
recurrence rate at the site of ablation is influenced by the size and
location of the metastatic lesions, as well as the use of percutaneous
vs laparoscopic approaches. Although local recurrence can often be
salvaged with repeat ablation or resection, for patients with limited
comorbidities in whom the goal is curative intent, surgical resection is
the preferred and most reliable method for actual cure. A meta-analysis
of nonrandomized studies comparing RFA with surgical resection
demonstrated an improvement in 5-year survival for patients treated with
hepatic resection.[20]
The
curative potential of surgical resection for hepatic metastases from
CRC varies depending on a number of important prognostic factors (Table
1). Nomograms for predicting cancer-related survival have been
developed, and may be helpful when considering the utility of
resection.[21] A patient’s risk for morbidity and mortality also plays a
significant role in defining the eventual treatment strategy. Surgical
resection is still associated with a defined mortality rate of 2.8% (0
to 6.6%), which is influenced, in large part, by the health of the
background liver.[22,23] Liver failure is the most common cause of death
after hepatectomy, and as discussed below, this complication is
influenced by the specific type and cumulative dose of chemotherapy
received. The indications for surgical resection are currently based on
feasibility and safety in patients who have responded to chemotherapy.
It is critically important for the surgical resection to leave 20% to
25% of functioning liver volume (future liver remnant [FLR]) in patients
with a normal background liver, and 40% of liver volume in patients
whose background liver is diseased from previous chemotherapy.[24]
Preoperative planning CT scans, including residual volume calculations,
are essential when planning an extended or bilobar resection.[25]
To
date, more than 750 series of hepatic metastasectomy for metastatic CRC
have been reported in the literature. The actuarial 5-year survival
rate for patients who underwent R0 resections (negative margins) was 30%
when combining 16 well-reported series of more than 100 patients with
follow-up greater than 2 years (15% to 67%).[22] While 5-year survival
was historically considered a cure for this disease, because of advances
in systemic chemotherapy an increasing number of patients are now
living with their disease beyond 5 years. A single-institution study of
455 patients revealed a median overall survival of 33 months, with 5-
and 10-year actuarial survival rates of 34% and 25%, respectively.[26]
In that study, 124 patients were identified as actual 5-year survivors
(27%), and of this group 59 were found to be 10-year survivors. This
finding suggests ongoing disease-related mortality beyond the 5-year
time-frame, with actual cure rates of 10% to 15%. Randomized clinical
data suggest an improvement in disease-free survival when systemic
chemotherapy is incorporated as part of a combined neoadjuvant and
postoperative adjuvant approach, as will be discussed in detail in this
article.
With the extended indications for hepatic metastasectomy
in the presence of active systemic chemotherapy, larger resections can
now be safely and effectively performed. Commonly used techniques
include staged resections for bilobar disease and preoperative portal
vein occlusion to achieve compensatory hypertrophy and safer extended
resections.[27,28] While there appear to be impressive actuarial 5-year
survival rates in these series of extensive surgical resections, it is
expected that the true cure rate will be much lower. When looking at
patients with initially unresectable colorectal liver metastases who
were treated with chemotherapy and then resected, 16% of this group were
considered cured, with a disease-free interval of more than 5 years
after metastasectomy.[29] On multivariate analysis, the main predictors
of cure included maximum size less than 3 cm, no more than three
metastatic lesions, and complete pathologic response.
Long-term cures
are exceedingly rare when patients with organ-limited mCRC are treated
with chemotherapy alone. In a retrospective review of 2751 patients with
metastatic CRC, during a median follow-up of 10.3 years, only 6 (0.24%)
were found to be free of disease after having received chemotherapy
alone.[30] It is now well established that a multimodality strategy
results in a much higher chance of long-term cure. In patients with
organ-limited disease, chemotherapy is administered in three main
settings, which include neoadjuvant therapy, conversion therapy, and
adjuvant therapy. Neoadjuvant therapy refers to chemotherapy given to
patients with potentially resectable disease, while conversion therapy
refers to chemotherapy given to patients deemed to have initially
unresectable disease. Adjuvant chemotherapy is use of chemotherapy
following an R0 surgical resection, with the intent of preventing
disease recurrence.
Up
to 20% to 30% of patients with liver-limited mCRC may have potentially
resectable disease at the time of initial presentation. However, because
a large proportion of patients experience recurrence of their disease
either in the liver or systemically, chemotherapy has been integrated in
their up-front care to improve upon the potential benefit of surgery.
Several clinical trials have specifically
evaluated the role of neoadjuvant therapy for patients with potentially
resectable liver metastases. In a single-arm trial involving 20
patients, neoadjuvant therapy with a weekly administration of FOLFOX
(fluorouracil [5-FU], leucovorin/folinic acid [LV], and
oxaliplatin(Drug information on oxaliplatin)
[Eloxatin]) resulted in a partial or complete response in all patients
enrolled.[31] A total of 16 patients underwent a potentially curative
resection, with 7 developing recurrence during the median follow-up
period of 23 months. A phase II trial of neoadjuvant therapy
investigated
bevacizumab(Drug information on bevacizumab) (Avastin) plus CapOx, the combination of
capecitabine(Drug information on capecitabine)
(Xeloda) and oxaliplatin.[32] In this study, 56 patients received 6
cycles of therapy prior to surgical resection, and a remarkably high
objective response rate of 73% was observed. A total of 52 of the 56
patients were able to undergo an R0 resection, with complete pathologic
response occurring in nearly 10% of patients. Given concerns over the
potential risks of bleeding or wound-healing complications, bevacizumab
was not given with the last cycle of chemotherapy prior to surgery. This
study is important as it showed that bevacizumab could be safely
administered to patients with no increased risk of intraoperative
bleeding or wound-healing complications. Moreover, it was estimated that
normal liver regeneration occurred in all but one patient.
The
European Organisation for Research and Treatment of Cancer (EORTC)
randomized phase III trial 40983 investigated use of perioperative
FOLFOX4 chemotherapy in patients with up to four resectable liver
metastases. In this study, patients were randomized to surgery alone or
to receive 6 cycles of FOLFOX4 before surgery and 6 cycles of FOLFOX4
after surgery.[33] The overall response rate was 43% in patients
receiving chemotherapy. Of note, surgery was performed in 83% of
patients randomized to chemotherapy and in 84% of patients randomized to
surgery alone, providing evidence that use of initial chemotherapy did
not compromise the ability of patients to undergo surgical resection.
While there was an increased risk of postoperative complications in
patients receiving neoadjuvant chemotherapy, these events were
reversible and not associated with an increased risk of mortality. When
the entire group of randomized patients was considered, a 7.3% increase
in progression-free survival (PFS) at 3 years was observed in patients
receiving chemotherapy, although this difference did not reach
statistical significance. However, in the group of patients who
underwent surgical resection, a significant 9.2% improvement in 3-year
PFS was, in fact, observed.
Adam et al examined the influence of
the response to neoadjuvant chemotherapy on the eventual outcome in
patients following surgical resection of multiple liver metastases.[34]
In this retrospective analysis of 131 patients, 44% underwent
hepatectomy after achieving an objective tumor response, 30% went to
surgical resection after tumor stabilization, and 26% were surgically
resected after tumor progression. Five-year survival was significantly
lower in the group of patients who had evidence of tumor progression,
compared with patients who had evidence of tumor response (8% vs 37%).
Of note, patients with stable disease on neoadjuvant chemotherapy had
only a slightly worse prognosis with respect to 5-year survival,
compared with responders (30% vs 37%). Disease-free survival in patients
who progressed on neoadjuvant chemotherapy was only 3%, compared with
rates of 21% and 20% for patients with tumor response or stable disease,
respectively. Based on this study, it is clear that tumor progression
before surgery is associated with extremely poor clinical outcome, and
in this setting, hepatic resection should be avoided in patients who are
deemed to be nonresponders to preoperative chemotherapy.
Neoadjuvant
chemotherapy may be associated with complete disappearance of some or
all of the hepatic metastases on imaging studies (approximately 18% of
tumors will disappear completely).[35] Pathological complete response is
associated with a high rate of long-term cure after surgical resection
(5-year survival of 79%).[36] Controversy exists regarding the need to
resect patients with complete radiographic responses, to achieve
long-term cure. Up to 70% of these sites of complete radiographic
response are associated with pathologic complete response or failure to
recur at these sites.[36,37] The remaining 30% of patients are at risk
of disease recurrence if resection is not performed. Thus, curative
therapy should include resection of these regions, although the
potential risk of disease recurrence at other sites must also be taken
into consideration.
The
majority of patients will present with liver metastases from CRC that
are unresectable or not optimally resectable based on their size,
number, or location at the time of initial assessment. In this setting,
conversion therapy is used in appropriately selected patients. The
primary focus, therefore, is on achieving downsizing of the metastatic
disease that is sufficient to allow surgical resection to be performed,
but not with the goal of achieving a complete or even maximal response.
Adam
and colleagues in France have had the largest experience in this area
to date, and their work has provided important insights into the
potential role of conversion therapy.[38-40] In their original series of
701 patients with initially unresectable liver metastases, treatment
with oxaliplatin-based chemotherapy resulted in downsizing in nearly 15%
of patients, and subsequent surgery. Based on 5-year follow-up after
surgery, 22% of patients had no evidence of residual or recurrent
disease. When stratified according to the underlying reasons for initial
unresectability, the 5-year overall survival (OS) rates were 60% for
patients with large tumors, 49% for those with poorly located tumors,
and 34% for patients with multinodular tumors. In an expanded series of
1439 patients treated with a broader range of cytotoxic chemotherapy,
the conversion rate was 12.5%, with a 5-year survival rate of 33%.
Folprecht
and colleagues[41] conducted an interesting analysis of all
published/presented clinical trials and retrospective studies of the
rate of objective response and the subsequent rate of resection of
initially unresectable metastases. They observed a strong correlation (r
= 0.96) between response rates and the subsequent resection rate in
patients with isolated liver disease. Moreover, their analysis confirmed
that patient selection and efficacy of preoperative chemotherapy were
strong predictors of potential resectability of liver metastases. Since
this analysis, several prospective clinical trials incorporating
systemic chemotherapy plus surgery have been performed. In these
studies, use of oxaliplatin- vs
irinotecan(Drug information on irinotecan)-based
chemotherapy has shown similar clinical outcomes.[42,43] Of note,
approximately 20% to 30% of patients were able to undergo R0 surgical
resection. Two trials have directly compared the clinical efficacy of
FOLFOX plus irinotecan (FOLFOXIRI), an aggressive regimen that
incorporates the three active cytotoxic agents, against that of FOLFIRI
(5-FU, LV, irinotecan). Falcone et al randomized patients with mCRC to
receive either FOLFOXIRI or FOLFIRI, and they reported a significant
increase in R0 resection for the subgroup of patients with liver-only
metastases who were randomized to the FOLFOXIRI arm.[44] The R0
resection rate was 36% in the FOLFOXIRI arm vs 12% in the FOLFIRI arm (
P
= .017). Despite the increased clinical activity of FOLFOXIRI, patients
receiving this regimen experienced a significantly higher incidence of
grade 3/4 toxicity in the form of myelosuppression and neurotoxicity. In
contrast to the positive findings of the Falcone study, Souglakos et al
observed a nonsignificant increase in overall response rate (43% vs
33.6%), conversion rate (10% vs 3.4%), and R0 resection rate (8.8% vs
3.4%).[45] A pooled analysis of the Falcone phase III study and two
phase II studies reported an overall response rate of 70% with the
FOLFOXIRI regimen and a 19% R0 resection rate. The 5-year disease-free
survival (DFS) and OS were 29% and 42%, respectively.[46]
Is
there an optimal cytotoxic chemotherapy regimen for conversion therapy?
To date, there has been a significant absence of randomized trials
directly comparing the various chemotherapy regimens in patients with
liver-limited disease. In reviewing the literature, it appears that
irinotecan- and oxaliplatin-based regimens yield approximately the same
rate of conversion, on the order of 20% to 30%. While FOLFOXIRI appears
to result in higher conversion rates, in the 40% to 60% range, and
higher R0 surgical resections, this treatment regimen is clearly
associated with increased toxicity and should be used only in certain
select patient populations. Upon review of the recent National
Comprehensive Cancer Institute (NCCN) guidelines, several regimens are
currently recommended, and they include FOLFIRI, FOLFOX, CapOx, and
FOLFOXIRI.[47]
The introduction of targeted therapies with either
the antiangiogenic agent bevacizumab or the epidermal growth factor
receptor (EGFR) inhibitors
cetuximab(Drug information on cetuximab)
(Erbitux) and panitumumab (Vectibix) has improved the clinical efficacy
of chemotherapy in patients with mCRC. As a result, combination
regimens incorporating these agents have now been evaluated in clinical
trials for patients with liver-limited metastases.
The addition
of the anti–vascular endothelial growth factor (VEGF) antibody
bevacizumab to either FOLFOX or to capecitabine and oxaliplatin
(XELOX/CapOx) vs the cytotoxic chemotherapy regimens alone was
investigated in a randomized phase III trial in advanced mCRC.[48]
Unfortunately, there was only a slightly higher incidence of R0 surgical
resection with bevacizumab (8.4%) vs chemotherapy alone (6.1%).
The
anti-EGFR antibodies cetuximab and panitumumab have been approved for
use in patients with mCRC.[49] Subsequent studies have shown that these
agents are active only in patients with wild-type
KRAS tumors.
KRAS mutations occur in up to 30% to 40% of patients with CRC, and they typically involve codon 12 or 13. In general,
KRAS
mutations lead to resistance to antibody therapy. However, recent
studies have suggested that the G13D mutation in codon 13 may still
allow for sensitivity to anti-EGFR antibody therapy, in sharp contrast
to mutations in codon 12.
Retrospective analyses of clinical
trials in mCRC have provided insights into the potential role of
cetuximab in the treatment of liver-limited disease. In a phase II trial
of FOLFOX plus cetuximab, 37 of the 43 patients enrolled had liver
involvement, and in 17 of these patients, the liver was the only site of
metastatic disease.[50] An objective response was seen in 34 of the 37
patients; 10 of these patients underwent surgical resection of their
metastases, including 8 patients with liver metastases. In a series of
151 patients with unresectable mCRC liver metastases refractory to
systemic chemotherapy, the addition of cetuximab to combination
chemotherapy allowed 27 patients to undergo surgical resection, and of
this group, 25 underwent potentially curative hepatectomy.[51] Of note,
this group included a majority of patients who were deemed to have
either technically unresectable or marginally resectable disease.
Moreover, the incorporation of cetuximab with chemotherapy conferred
significant clinical benefit, with median progression-free survival
(PFS) and OS of 13 and 20 months, respectively.
Several
single-arm phase II trials have investigated the combination of
cetuximab with either irinotecan- or oxaliplatin-based regimens. Min et
al reported a radiologic response rate of 39%, with 30% of patients
treated with FOLFIRI plus cetuximab able to undergo resection of their
liver metastases.[52] Nearly identical results were observed with the
combination of FOLFOX and cetuximab, which yielded an R0 resection rate
of 29%.[53]
Two recent randomized studies have investigated the
safety and efficacy of cetuximab in combination with either FOLFIRI[54]
or FOLFOX.[55] The addition of cetuximab to FOLFIRI significantly
increased the overall response rate (59% vs 43%;
P = .004) in patients with wild-type
KRAS when
compared with FOLFIRI alone, and this resulted in a higher number of
patients able to undergo R0 surgical resection (4.3% vs 1.5%). An
exploratory analysis revealed a two-fold higher rate of R0 surgical
resection in patients with liver-limited disease (9.8% vs 4.5%).[54]
Similar findings were reported by Bokemeyer et al[55] with the
combination of cetuximab plus FOLFOX4. The overall response rate
increased from 37% to 61% in patients with wild-type
KRAS and in
those treated with the combination vs FOLFOX4 alone. This improvement in
response rate in patients treated with the combination was associated
with an increase in the R0 resection rate from 2.4% to 4.7%.
A
trial of 114 patients with initially nonresectable liver-limited
metastases randomized patients to receive cetuximab in combination with
either FOLFOX6 or FOLFIRI. R0 resection rates of 38% and 30% were
observed, respectively, with an overall R0 resection rate of 34%.[56] In
a retrospective analysis of response according to
KRAS status with the two arms of the trial combined, the clinical response rate in patients with wild-type
KRAS was 70% compared with 41% for those with mutant
KRAS.
This study provides further evidence of the strong association between
high tumor response rate and increased rate of liver metastasectomy.
PRIME
(the Panitumumab Ran-domized Trial in Combination With Chemotherapy for
Metastatic Colorectal Cancer to Determine Efficacy) was designed to
evaluate the efficacy and safety of panitumumab plus FOLFOX4 vs FOLFOX4
alone as initial treatment for mCRC. The addition of panitumumab to
FOLFOX4 chemotherapy significantly improved the overall response rate
(57% vs 48%;
P = .02) and median PFS in patients with wild-type
KRAS tumors (9.6 vs 8.0 months;
P = 0.01), which translated into a nonsignificant increase in median OS from 19.7 to 23.9 months.
In
terms of surgical resection, metastasectomy of any site was attempted
in 10.5% of patients treated with the combination regimen as opposed to
9.4% of patients treated with chemotherapy alone. However, the R0
resection rate was higher in patients with wild-type
KRAS tumors
and liver-limited disease (28% vs 18%) who were treated with panitumumab
plus FOLFOX4. At the time of the most recent analysis, median OS had
not been reached in patients who underwent R0 liver resection, in
contrast to a median OS of 23.6 months in those who were unable to
undergo complete surgical resection.[57]
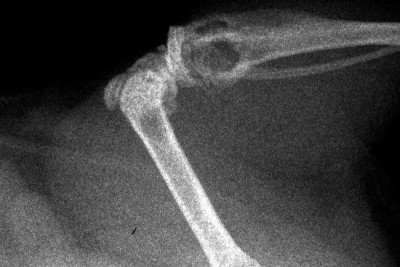 This X-ray image shows metastatic bone
tumors in a mouse with kidney cancer. The metastatic tumors appear as
hollow or dark areas in the bones.
This X-ray image shows metastatic bone
tumors in a mouse with kidney cancer. The metastatic tumors appear as
hollow or dark areas in the bones.












