ASIDE FROM THOSE INCORPORATED IN THE GUIDELINES OF ONCOLOGY PRACTICE
1.EGFR
2.ALK
Now we are hearing about the following
1.ROS-1
2.MEK-1
3.RET
4.BRAF
5.HER-2
6.PI3KCA
7.KRAS
8.PD-1,2
9.ERCC1
10.BRCA-1 mRNA
11 P53
What about the therapeutic roles of :
GSTM-1 and GSTT1,FAK, Wnt, Notch, p16,
HIF and VGEF and the CYP1A1,P ?
A blog about research, awareness, prevention, treatment and survivorship of Breast Cancer and all cancers, including targeted scientific research and a grassroots approach to increase screening for cancer, especially in the low income and under-insured population of El Paso, Texas, with a view to expand this new health care model to many other 'minority' populations across the United States and beyond
Showing posts with label P53. Show all posts
Showing posts with label P53. Show all posts
Thursday, November 14, 2013
NEW GENES ARE BEING INCLUDED IN THE CLINICAL THERAPY OF LUNG CANCERS!
Labels:
16,
BRCA-1 mRNA,
crbcm,
CYP1A1,
ERCC1,
FAK,
GSTM-1,
GSTT1,
HIF,
kankonde,
KRAS,
lung cancer,
notch,
P53,
PI3KCA,
VGEF,
Wnt
Saturday, November 9, 2013
CLINICAL ASPECTS OF HIV INFECTION
The HIV challenge has many interesting aspects when it comes to pathophysiology and genetic based studies. It goes without saying that the disease is bad and has caused many deplorable deaths. But for scientists it has provided significant opportunity for advances as it has shed light on several aspects of this disease:
1. Viral infection: the takeover of the Human genome to the benefit of the life of the Virus
2. Sexually transmitted diseases and difficulties in controlling this line of infections, particularly in poor populations
3. Impact of hormone (Testosterone and corticoids which tend to worsen the disease such as in Kaposi Sarcoma)
4. Revealing weaknesses in the structure of our Immune systems for the decrease of CD4, to the development of lymphoproliferative disorders, to the development of opportunistic infections, to the increased risk of AIDS related lymphomas (ARL) in patients expressing Stromal cell derived Factor 1 ( and decrease risk in those having a deletion in Chemokine Receptor CCR5)
5. On the genetic front, Mutations, suppression and translocations of the c-MYC, P53, and Bcl6...
6. The disease causes the body to be swamped with Cytokines ( IL-1,6,10)
7. The disease has shown us the importance of duration of exposure as various diseases develop the longer you stay under the curb of low CD4 (less than 100) with certain diseases being seen only at certain CD4 counts.
8. New biomarkers are now defined CD30 (heightened risk of progression of ARL)
and new diagnosis (CD138, VS38c for Plasmablastic lymphoma)
9. Early introduction of Etoposide in the treatment plan seems to be important with the resurgence of the EPOCH regimen rather than CHOP; Etoposide seems to control those Epigenetic events better!
10. Eminence of Macrophages in the inflammatory process as they drive the EGFR
and the use of Anti-VEGF in KS. An angiosarcoma...(where is Avastin?)
You name HIV, the syndrome does it. The push for us is to go back to the genetic bases of this disease!
1. Viral infection: the takeover of the Human genome to the benefit of the life of the Virus
2. Sexually transmitted diseases and difficulties in controlling this line of infections, particularly in poor populations
3. Impact of hormone (Testosterone and corticoids which tend to worsen the disease such as in Kaposi Sarcoma)
4. Revealing weaknesses in the structure of our Immune systems for the decrease of CD4, to the development of lymphoproliferative disorders, to the development of opportunistic infections, to the increased risk of AIDS related lymphomas (ARL) in patients expressing Stromal cell derived Factor 1 ( and decrease risk in those having a deletion in Chemokine Receptor CCR5)
5. On the genetic front, Mutations, suppression and translocations of the c-MYC, P53, and Bcl6...
6. The disease causes the body to be swamped with Cytokines ( IL-1,6,10)
7. The disease has shown us the importance of duration of exposure as various diseases develop the longer you stay under the curb of low CD4 (less than 100) with certain diseases being seen only at certain CD4 counts.
8. New biomarkers are now defined CD30 (heightened risk of progression of ARL)
and new diagnosis (CD138, VS38c for Plasmablastic lymphoma)
9. Early introduction of Etoposide in the treatment plan seems to be important with the resurgence of the EPOCH regimen rather than CHOP; Etoposide seems to control those Epigenetic events better!
10. Eminence of Macrophages in the inflammatory process as they drive the EGFR
and the use of Anti-VEGF in KS. An angiosarcoma...(where is Avastin?)
You name HIV, the syndrome does it. The push for us is to go back to the genetic bases of this disease!
Saturday, November 2, 2013
Critical importance of the Notch1
TSG1, HGS, and STAM2 appear critical in the importance of the NOTCH1.
We have stressed the importance of the NOTCH in cancer and wanted to provide some of the proof for the supportive evidence found in the literature. The Notch through its interaction with MAML1, easily affects EP300 leading to activation of TSG, a critical gene in the action of P53. Indeed P53 acts by activating TSG which leads to an increasing inhibitory activity of p21 on CDKs, blocking as a result cell division and therefore proliferation.
Inhibition at the NOTCH will therefore remove breaks to cell division and will mark a significant tendency to cancer incurability!
And I wish things stop there, but they don't:
The Activation of TSG will disturb the resting HSG which bothers the Merlin and blocks NF2 leading to the loss of growth control by contact of surrounding cells, the cell losing control of its growth...Hyperplasia can easily ensue!
The HSG now excited, engages the STAM2 and 3 things:
1. Interaction with JAK1 leading to metastasis
" Expression of JAK1 in cancer cells enables individual cells to contract, potentially allowing them to escape their tumor and metastasize to other parts of the body (wikipedia)"
the involvement of JAK-1 multiply the worsening of the situation because it will excite: PTPN11
" PTPN11 is a member of the protein tyrosine phosphatase (PTP) family. PTPs are known to be signaling molecules that regulate a variety of cellular processes including cell growth, differentiation, mitotic cycle, and oncogenic transformation."
and with the ELP gene, the process will affect the SMAD3 leading to loss of control of proliferation and normal ubiquitylation of inhibitory proteins.
2.S TAM2 will engage Cytokin Receptors (Cullins)
3. STAM2 will engage the tract to E3.
But the engagement of the Notch does still not stop there...
the GSK3B comes into play! and ....
We have stressed the importance of the NOTCH in cancer and wanted to provide some of the proof for the supportive evidence found in the literature. The Notch through its interaction with MAML1, easily affects EP300 leading to activation of TSG, a critical gene in the action of P53. Indeed P53 acts by activating TSG which leads to an increasing inhibitory activity of p21 on CDKs, blocking as a result cell division and therefore proliferation.
Inhibition at the NOTCH will therefore remove breaks to cell division and will mark a significant tendency to cancer incurability!
And I wish things stop there, but they don't:
The Activation of TSG will disturb the resting HSG which bothers the Merlin and blocks NF2 leading to the loss of growth control by contact of surrounding cells, the cell losing control of its growth...Hyperplasia can easily ensue!
The HSG now excited, engages the STAM2 and 3 things:
1. Interaction with JAK1 leading to metastasis
" Expression of JAK1 in cancer cells enables individual cells to contract, potentially allowing them to escape their tumor and metastasize to other parts of the body (wikipedia)"
the involvement of JAK-1 multiply the worsening of the situation because it will excite: PTPN11
" PTPN11 is a member of the protein tyrosine phosphatase (PTP) family. PTPs are known to be signaling molecules that regulate a variety of cellular processes including cell growth, differentiation, mitotic cycle, and oncogenic transformation."
and with the ELP gene, the process will affect the SMAD3 leading to loss of control of proliferation and normal ubiquitylation of inhibitory proteins.
2.S TAM2 will engage Cytokin Receptors (Cullins)
3. STAM2 will engage the tract to E3.
But the engagement of the Notch does still not stop there...
the GSK3B comes into play! and ....
Thursday, August 22, 2013
Processes of cancerization
One of the most intriguing steps in the neoplastic transformation is determining the actual event that led to its occurrence. We all have the perception that because of what we ingest unfortunately on a continuous basis (medications or foods we like - man clings to habits) something will get either amplified or suppressed. Certain amplifications can be deleterious or beneficial depending of where they occur or what gene is involved. It is apparent that involvement of "wild genes" (those with multiple interactions with others, including genes involved in shaping the body) are more likely to lead to malignant transformation (ie. the Androgen gene, FYN,Grb2, MTIF, etc). Secondly, knocking out break to proliferation (P53, Rb1, PTEN, and the many CDK) seems also to be a prelude to a neoplastic transformation. Alteration in "switch" genes (SOS) and molecules intermediary to various cellular/membrane events can also trigger a persistent stimulation or suppression that could affect cellular processes enough to upset a balance. Chronic hypoxia has emerged to be a potent neoplastic process inducer....(to be continued)
Labels:
cancerization,
CDK,
chronic hypoxia,
crbcm,
FYN,
gene amplification,
gene suppression,
Grb2,
MTIF,
P53,
PTEN,
RB1,
SOS,
wild genes
A few questions in triple negative breast cancer
1.Could amplification of PIAS modulate enough the STAT to impact progression of triple negative Breast cancer?
2.Could modifiers of Sumoylation impact the prognosis of triple negative breast cancer?
3.Status of the Zimp10 in triple negative breast cancer?
4. Amplifying ART-27 to stop cellular proliferation?
5.blocking RCHY1 could restore P53 function in patient with non Mutated P53?
6.can anti-cortactin and supervillin block metastatic propensity of triple negative breast cancers?
watch brain mets?
2.Could modifiers of Sumoylation impact the prognosis of triple negative breast cancer?
3.Status of the Zimp10 in triple negative breast cancer?
4. Amplifying ART-27 to stop cellular proliferation?
5.blocking RCHY1 could restore P53 function in patient with non Mutated P53?
6.can anti-cortactin and supervillin block metastatic propensity of triple negative breast cancers?
watch brain mets?
Thursday, April 25, 2013
NEW OPTIMISM IN RECURRENT OVARIAN CANCER
" There is reason to be optimistic about the future of therapy for
patients with recurrent ovarian cancer. Inhibition of Wee-1 may target
the universal p53 aberrations observed in high-grade serous
cancers, and Wee-1 inhibitors are being developed. Objective responses
to a variety of immune therapies have been observed, such as an antibody
against cytotoxic T-lymphocyte protein 4 (CTLA 4) (see reference 66
from Vaughn et al[9]) or BMS-936559, and antiprogrammed death ligand-1
(PDL-1) monoclonal antibody[15] and immune therapies are a promising
area for development. Aberrant DNA methylation is a frequent epigenetic
event in ovarian cancer, and the use of chemotherapy plus epigenetic
modulators such as demethylating agents or histone deacetylase
inhibitors is being studied. The ability to analyze complex genomic data
is rapidly increasing, and ovarian cancer is fairly readily biopsiable.
More than ever, patients with recurrent disease should consider
participation in high quality research trials."
"the addition of PARP inhibitors to chemotherapy in women with recurrent disease has so far failed to improve survival.[14] Front-line trials with PARP inhibitors are being planned, and may yield better results"
FROM:
Management of Recurrent EOC: The State of the Art
WE ARE GOING TO FURTHER COMMENTS OF THESE NEW OPTIONS AS WE LEARN MORE!
MAY BE WE SHOULD BE ADDING INHIBITORS OF AURORA (s) INSTEAD !
"the addition of PARP inhibitors to chemotherapy in women with recurrent disease has so far failed to improve survival.[14] Front-line trials with PARP inhibitors are being planned, and may yield better results"
FROM:
Management of Recurrent EOC: The State of the Art
By Gini F. Fleming, MD1 |
April 15, 2013
---------------------------------------------------------------------------------------WE ARE GOING TO FURTHER COMMENTS OF THESE NEW OPTIONS AS WE LEARN MORE!
MAY BE WE SHOULD BE ADDING INHIBITORS OF AURORA (s) INSTEAD !
Saturday, March 16, 2013
THE AURORA KINASES
ONCE AGAIN YOU SEE HOW THE CELL PLAYS, USING SIMPLE THINGS THAT GET COMPLICATED REALLY QUICKLY!
Given our current understanding of the way they are suppressed by normal activity of P53, the aurora Kinase inhibitors should be used in cancers where P53 is clearly dys-regulated, and probably in disease with positive Prostate Stem Cell Antigen. This open the door to Sarcomas (chondrosarcoma being the most cited) and Pancreatic cancers (as well as Bladder cancers).
GADD45, a P53 dependent protein that inhibits Cdc2/Cyclin B1 could therefore be the best predictor of Aurora activity.
Quantification of CDCA8/Borealin, BIRC5/survivin, and INCENP may provide additional information on AURORA KINASE ACTIVITY. Like the core Binding Factor, these 3 Molecules form the Chromosomal Passenger Complex (CPC) which interact with POGZ, EVI5, and JTB.
Niehrs at al further define the role of GADD45 as "Gadd45 recruits nucleotide and/or base excision repair factors to gene-specific loci and acts as an adapter between repair factors and chromatin, thereby creating a nexus between epigenetics and DNA repair." Therefore explaining how P53 induced arrest is followed by DNA repair through recruitment of GADD45. When the cell is trying to repair itself with increase in GADD45, of course it wont want to die, therefore over-expression of GADD45 decrease the c-JUN, protecting therefore from TNF induced apoptosis. GADD45 is not good theoretically when you use Cisplatin or radiation for that matter!
*POGZ explains Nuclear transposition of P53 effects as it impacts SP1, a transcription factor with inteaction of all major playors in the cell including E2F1, POU2F1. YOU TARGET SP1 WITH WITH AFERIN FOR EXAMPLE, IT IS IMPOSSIBLE TO COME UP EMPTY HANDED.
*EVI5
"Identification of Rab11 as a small GTPase binding protein for the Evi5 oncogene"
Protein JTB also known as the jumping translocation breakpoint protein or prostate androgen-regulated protein (PAR) is a protein that in humans is encoded by the JTB gene.[1][2]
The JTB family of proteins contains several jumping translocation breakpoint proteins or JTBs. Jumping translocation (JT) is an unbalanced translocation that comprises amplified chromosomal segments jumping to various telomeres. JTB has been found to fuse with the telomeric repeats of acceptor telomeres in a case of JT. Homo sapiens JTB (hJTB) encodes a transmembrane protein that is highly conserved among divergent eukaryotic species. JT results in a hJTB truncation, which potentially produces an hJTB product devoid of the transmembrane domain. hJTB is located in a gene-rich region at 1q21, called EDC (Epidermal Differentiation Complex).[1] JTB has also been implicated in prostatic carcinomas.[3]
KANOME ET AL SUGGESTED
"JTB-induced clustering of mitochondria around the nuclear periphery and swelling of each mitochondrion. In those mitochondria, membrane potential, as monitored with a JC-1 probe, was significantly reduced. Coinciding with these changes in mitochondria, JTB retarded the growth of the cells and conferred resistance to TGF- 1-induced
apoptosis. These activities were dependent on the N-terminal processing
and induced by wild-type JTB but not by a mutant resistant to cleavage.
These findings raised the possibility that aberration of JTB in
structure or expression induced neoplastic changes in cells through
dysfunction of mitochondria leading to deregulated cell growth and/or
death."
1-induced
apoptosis. These activities were dependent on the N-terminal processing
and induced by wild-type JTB but not by a mutant resistant to cleavage.
These findings raised the possibility that aberration of JTB in
structure or expression induced neoplastic changes in cells through
dysfunction of mitochondria leading to deregulated cell growth and/or
death."
==================================================================
ONCE AGAIN YOU SEE HOW THE CELL PLAYS, USING SIMPLE THINGS THAT GET COMPLICATED REALLY QUICK!
Given our current understanding of the way they are suppressed by normal activity of P53, the aurora Kinase inhibitors should be used in cancers where P53 is clearly dys-regulated, and probably in disease with positive Prostate Stem Cell Antigen. This open the door to Sarcomas (chondrosarcoma being the most cited) and Pancreatic cancers (as well as Bladder cancers).
GADD45, a P53 dependent protein that inhibits Cdc2/Cyclin B1 could therefore be the best predictor of Aurora activity.
Quantification of CDCA8/Borealin, BIRC5/survivin, and INCENP may provide additional information on AURORA KINASE ACTIVITY. Like the core Binding Factor, these 3 Molecules form the Chromosomal Passenger Complex (CPC) which interact with POGZ, EVI5, and JTB.
Niehrs at al further define the role of GADD45 as "Gadd45 recruits nucleotide and/or base excision repair factors to gene-specific loci and acts as an adapter between repair factors and chromatin, thereby creating a nexus between epigenetics and DNA repair." Therefore explaining how P53 induced arrest is followed by DNA repair through recruitment of GADD45. When the cell is trying to repair itself with increase in GADD45, of course it wont want to die, therefore over-expression of GADD45 decrease the c-JUN, protecting therefore from TNF induced apoptosis. GADD45 is not good theoretically when you use Cisplatin or radiation for that matter!
*POGZ explains Nuclear transposition of P53 effects as it impacts SP1, a transcription factor with inteaction of all major playors in the cell including E2F1, POU2F1. YOU TARGET SP1 WITH WITH AFERIN FOR EXAMPLE, IT IS IMPOSSIBLE TO COME UP EMPTY HANDED.
*EVI5
"Identification of Rab11 as a small GTPase binding protein for the Evi5 oncogene"
This article has been cited by other articles in PMC.
Abstract
The Evi5 oncogene has recently been shown to regulate the stability and accumulation of critical G1
cell cycle factors including Emi1, an inhibitor of the
anaphase-promoting complex/cyclosome, and cyclin A. Sequence analysis of
the amino terminus of Evi5 reveals a Tre-2, Bub2, Cdc16 domain, which
has been shown to be a binding partner and GTPase-activating protein
domain for the Rab family of small Ras-like GTPases. Here we describe
the identification of Evi5 as a candidate binding protein for Rab11, a
GTPase that regulates intracellular transport and has specific roles in
endosome recycling and cytokinesis. By yeast two-hybrid analysis,
immunoprecipitation, and Biacore analysis, we demonstrate that Evi5
binds Rab11a and Rab11b in a GTP-dependent manner. However, Evi5
displays no activation of Rab11 GTPase activity in vitro. Evi5 colocalizes with Rab11 in vivo,
and overexpression of Rab11 perturbs the localization of Evi5,
redistributing it into Rab11-positive recycling endosomes.
Interestingly, in vitro binding studies show that Rab11
effector proteins including FIP3 compete with Evi5 for binding to Rab11,
suggesting a partitioning between Rab11–Evi5 and Rab11 effector
complexes. Indeed, ablation of Evi5 by RNA interference causes a
mislocalization of FIP3 at the abscission site during cytokinesis. These
data demonstrate that Evi5 is a Rab11 binding protein and that Evi5 may
cooperate with Rab11 to coordinate vesicular trafficking, cytokinesis,
and cell cycle control independent of GTPase-activating protein
function.
Keywords: cytokinesis, GTPase-activating protein, recycling endosome".
*JTB
JTB (gene)
From Wikipedia, the free encyclopedia
Jump to: navigation, search
| Jumping translocation breakpoint | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
|
|||||||||||
| Identifiers | |||||||||||
| Symbols | JTB; HJTB; HSPC222; PAR; hJT | ||||||||||
| External IDs | OMIM: 604671 MGI: 1346082 HomoloGene: 4870 GeneCards: JTB Gene | ||||||||||
|
|||||||||||
| RNA expression pattern | |||||||||||
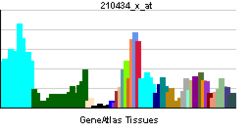 |
|||||||||||
 |
|||||||||||
| More reference expression data | |||||||||||
| Orthologs | |||||||||||
| Species | Human | Mouse | |||||||||
| Entrez | 10899 | 23922 | |||||||||
| Ensembl | ENSG00000143543 | ENSMUSG00000027937 | |||||||||
| UniProt | O76095 | O88824 | |||||||||
| RefSeq (mRNA) | NM_006694 | NM_206924 | |||||||||
| RefSeq (protein) | NP_006685 | NP_996807 | |||||||||
| Location (UCSC) | Chr 1: 153.95 – 153.95 Mb |
Chr 3: 90.23 – 90.24 Mb |
|||||||||
| PubMed search | [1] | [2] | |||||||||
| Jumping translocation breakpoint protein (JTB) | |||
|---|---|---|---|
| Identifiers | |||
| Symbol | JTB | ||
| Pfam | PF05439 | ||
| InterPro | IPR008657 | ||
|
|||
The JTB family of proteins contains several jumping translocation breakpoint proteins or JTBs. Jumping translocation (JT) is an unbalanced translocation that comprises amplified chromosomal segments jumping to various telomeres. JTB has been found to fuse with the telomeric repeats of acceptor telomeres in a case of JT. Homo sapiens JTB (hJTB) encodes a transmembrane protein that is highly conserved among divergent eukaryotic species. JT results in a hJTB truncation, which potentially produces an hJTB product devoid of the transmembrane domain. hJTB is located in a gene-rich region at 1q21, called EDC (Epidermal Differentiation Complex).[1] JTB has also been implicated in prostatic carcinomas.[3]
KANOME ET AL SUGGESTED
"JTB-induced clustering of mitochondria around the nuclear periphery and swelling of each mitochondrion. In those mitochondria, membrane potential, as monitored with a JC-1 probe, was significantly reduced. Coinciding with these changes in mitochondria, JTB retarded the growth of the cells and conferred resistance to TGF-
 1-induced
apoptosis. These activities were dependent on the N-terminal processing
and induced by wild-type JTB but not by a mutant resistant to cleavage.
These findings raised the possibility that aberration of JTB in
structure or expression induced neoplastic changes in cells through
dysfunction of mitochondria leading to deregulated cell growth and/or
death."
1-induced
apoptosis. These activities were dependent on the N-terminal processing
and induced by wild-type JTB but not by a mutant resistant to cleavage.
These findings raised the possibility that aberration of JTB in
structure or expression induced neoplastic changes in cells through
dysfunction of mitochondria leading to deregulated cell growth and/or
death."==================================================================
ONCE AGAIN YOU SEE HOW THE CELL PLAYS, USING SIMPLE THINGS THAT GET COMPLICATED REALLY QUICK!
Labels:
aurora kinases,
bladder cancer,
borealin,
CDC2,
CDCA8,
chondrosarcoma,
cisplatin,
crbcm,
Cyclin B1,
dysregulation,
kinase inhibitors,
P53,
pancreatic cancer,
prostate stem cell antigen,
sarcoma
Sunday, March 3, 2013
Smooth Muscle Myosin & Leukemia
1.SMMHC, a Smooth Muscle Myosin related marker of differentiation, but
also implying the use of multiple regulatory genes that ultimately depress P53
as a way to decrease repair of DNA and allow leukemia to proceed with
proliferation. this marker is seen in Inv-16 Leukemia. Through
interaction with SMAD3, it affects TGF driven migration of leukemic
cells. It also interfere with ACTA 2, TGFBR-2 AND FBN-1,
THIS SUGGEST THAT BLOCKING MIGRATION AND IMMUNE BETA-2 RECEPTOR OF TGF COULD ADD TO ACUTE EOSINOPHILIC LEUKEMIA. BLOCKING NUCLEAR INTERNALIZATION OF THE BETA SUBUNIT OF THE CBF WOULD HELP IN THE CBF DRIVEN LEUKEMIA IN GENERAL.
2.HOXD3
" Mutations in this particular gene cause synpolydactyly and Brachydactyly. The product of the mouse Hoxd13 gene plays a role in axial skeleton development ...
remember the role of Anti-VEGF /MEK in people with gene that impairs morphogenesis. leukemia with this mutation could a get a trial!
3 MEIS, a cofactor to the "soul of AML" E3
remember we discussed the AML is characterized by suppression of NF-kB
that suppression is achieved by this MEIS over-expression. it is the over expression to
HOS protein which is
'The homologue of Slimb (HOS) F-box protein is a receptor of the Skp1-Cullin1-F-box protein (SCF(HOS)) E3 ubiquitin ligase, which mediates ubiquitination and degradation of beta-catenin and the inhibitor of NFkappaB, IkappaB.''
You block this stuff, you release NF-kB, you slow down leukemia or at least decrease co-existing infection rates (role in transplant patients).
THIS SUGGEST THAT BLOCKING MIGRATION AND IMMUNE BETA-2 RECEPTOR OF TGF COULD ADD TO ACUTE EOSINOPHILIC LEUKEMIA. BLOCKING NUCLEAR INTERNALIZATION OF THE BETA SUBUNIT OF THE CBF WOULD HELP IN THE CBF DRIVEN LEUKEMIA IN GENERAL.
2.HOXD3
" Mutations in this particular gene cause synpolydactyly and Brachydactyly. The product of the mouse Hoxd13 gene plays a role in axial skeleton development ...
remember the role of Anti-VEGF /MEK in people with gene that impairs morphogenesis. leukemia with this mutation could a get a trial!
3 MEIS, a cofactor to the "soul of AML" E3
remember we discussed the AML is characterized by suppression of NF-kB
that suppression is achieved by this MEIS over-expression. it is the over expression to
HOS protein which is
'The homologue of Slimb (HOS) F-box protein is a receptor of the Skp1-Cullin1-F-box protein (SCF(HOS)) E3 ubiquitin ligase, which mediates ubiquitination and degradation of beta-catenin and the inhibitor of NFkappaB, IkappaB.''
Stability of homologue of Slimb F-box protein is regulated by availability of its substrate.
You block this stuff, you release NF-kB, you slow down leukemia or at least decrease co-existing infection rates (role in transplant patients).
Thursday, January 10, 2013
TRIPLE NEGATIVE BREAST CANCER, A MELTING POT
The news that the Genome of triple negative breast cancer is similar to ovarian cancer has been good as a starting point. But that is as far as it goes! Researcher are now scrambling trying to see how to best use this information and there is not one good direction. In fact if anything, it may have complicated the landscape.
The controversy is compounded by the news that there is not simply a single type of Triple Negative Breast cancer. This added to the fact that there is not just one type of Ovarian cancer. So which one is the best approach? And there are no known good suggestions, because of a lack of comprehensive database for cancer types. Our cancer knowledge is disconnected. Someone knows more about this. Someone else knows about that. There are Gaps in the knowledge which prevents us from moving forward.
Some of the facts and knowledge:
1. That the Genome is similar to Ovarian Cancer.
2. That Taxane-Cisplatin works in Ovarian Cancer
3. That PARP may have a role
4. That (low) MEKK1 expression is linked to tumor Response to Cisplatin.
5. That BRAC may impart a poor prognosis to the tumor
6. That Downregulation of STAT1 may play a role in the Oncogenesis of Triple Negative Breast cancer.
7. The almost total lack of Role of P53 alteration
8. Limited role of Kras Mutation
etc.
There are Major Questions of therapeutic importance:
1.Are these cancers MUCINOUS? Is there presence of MUC family members?
If these tumors are mucinous, this is another bad news. Mucin presence shields against detection by the innate immune system and favors cancer dissemination to go undetected. Mucin contains molecules that interfere with Glycocalyx, blunting their ability to expose cancer cells to the immune system, and also contain molecules full of Sulfhydryl expressing molecules which have profound interaction with electron based reactions at the membrane and Intracellularly. These activities are generally protective for the cancer cell.
The Mucinous presence can also be supported by the presence of Galectin 4 (LGALS4) 19q13.3 (Heterozygosity site). Positive TFF1 of the trefoil factor family which is an Estrogen regulated molecule that could potentially predict some response to hormone manipulation even in triple negative setting.
Amplification of CDX which modulate proliferation, cell adhesion and Apoptosis. The fact is this CDX could be a driver phenomena as this cancer is known for its ability to have a steady progression.
OTHER Molecules of Importance CDH17, Tetraspanin, MSF1R, E-Cadherin and the Kruppel like factor.
2. These tumors seems to have a survival that is epic, raising the issue of expression of survival pathways MEK, MAP Kinases and C-jun
3. What differentiates Endometrioid Vs other ovarian cancers will play a role in this disease
4. What is the role of target therapy, important in Ovarian cancer, as it relates to Triple negative breast cancer?
We are only just scratching the surface of this problem,
Time to put the puzzle together!
The news that the Genome of triple negative breast cancer is similar to ovarian cancer has been good as a starting point. But that is as far as it goes! Researcher are now scrambling trying to see how to best use this information and there is not one good direction. In fact if anything, it may have complicated the landscape.
The controversy is compounded by the news that there is not simply a single type of Triple Negative Breast cancer. This added to the fact that there is not just one type of Ovarian cancer. So which one is the best approach? And there are no known good suggestions, because of a lack of comprehensive database for cancer types. Our cancer knowledge is disconnected. Someone knows more about this. Someone else knows about that. There are Gaps in the knowledge which prevents us from moving forward.
Some of the facts and knowledge:
1. That the Genome is similar to Ovarian Cancer.
2. That Taxane-Cisplatin works in Ovarian Cancer
3. That PARP may have a role
4. That (low) MEKK1 expression is linked to tumor Response to Cisplatin.
5. That BRAC may impart a poor prognosis to the tumor
6. That Downregulation of STAT1 may play a role in the Oncogenesis of Triple Negative Breast cancer.
7. The almost total lack of Role of P53 alteration
8. Limited role of Kras Mutation
etc.
There are Major Questions of therapeutic importance:
1.Are these cancers MUCINOUS? Is there presence of MUC family members?
If these tumors are mucinous, this is another bad news. Mucin presence shields against detection by the innate immune system and favors cancer dissemination to go undetected. Mucin contains molecules that interfere with Glycocalyx, blunting their ability to expose cancer cells to the immune system, and also contain molecules full of Sulfhydryl expressing molecules which have profound interaction with electron based reactions at the membrane and Intracellularly. These activities are generally protective for the cancer cell.
The Mucinous presence can also be supported by the presence of Galectin 4 (LGALS4) 19q13.3 (Heterozygosity site). Positive TFF1 of the trefoil factor family which is an Estrogen regulated molecule that could potentially predict some response to hormone manipulation even in triple negative setting.
Amplification of CDX which modulate proliferation, cell adhesion and Apoptosis. The fact is this CDX could be a driver phenomena as this cancer is known for its ability to have a steady progression.
OTHER Molecules of Importance CDH17, Tetraspanin, MSF1R, E-Cadherin and the Kruppel like factor.
2. These tumors seems to have a survival that is epic, raising the issue of expression of survival pathways MEK, MAP Kinases and C-jun
3. What differentiates Endometrioid Vs other ovarian cancers will play a role in this disease
4. What is the role of target therapy, important in Ovarian cancer, as it relates to Triple negative breast cancer?
We are only just scratching the surface of this problem,
Time to put the puzzle together!
TAXOTERE-CISPLATIN SUPERIOR TO TAXOTERE-XELODA IN TRIPLE NEGATIVE BREAST CANCER
In a recent article published in the Annals of Oncology, Researcher published that Taxotere Cisplatin was a better combination for initial therapy in Metastatic triple negative breast cancer:
"Results:
"Results:
- The median follow-up was 24 months. ORR was higher in the TP group than in the TX group (63.0% versus 15.4%, P = 0.001).
- PFS was more than doubled (10.9 months versus 4.8 months, P < 0.001) and median OS was also greatly improved (32.8 months versus 21.5 months, P = 0.027).
- Toxic effects were not different except G3/4 vomiting and G2/3 hand-foot syndrome.
These results corroborate or tend to support many facts:
1. That triple negative Breast cancer genome was closer to ovarian cancer, a disease in which Taxol -Carboplatin is still standard of care particularly in metastatic setting.
2. That Cisplatin alteration of DNA is more likely to induce P53 cell cycle arrest. (1st law)
3. That adding Taxotere and its disruption of Macrotubules recruits effectively the 2nd law. This lead to a doubling of PROGRESSION FREE SURVIVAL.
Again it would be of interest to see what an Anti-kinesin (anti-Actin) or Velcade addition would mean in a clinical trial. Most molecules involved in programmed cell death such as Cytochrome C are attached to membrane within the organel where they reside. Disrupting that anchor would most likely boost Apoptosis. Without further determining the nature of that Anchor, we know that the cytoskeleton is most likely Actinic in nature. Disruption of the the Cytoskeleton could induced Anoikis, and freedom of molecules attached to membranes leading to major disruption including that of signal pathways.
Velcade main additional effect is disruption of DNA replication restarting after P53 arrest by its affect anti-proteasomic. Protein restarting the replication are generally ubiquitinated making the front and center to proteasome role! The issue really remains the determination of how much of a Driver this pathway is in solid tumor. This determination is one of the major challenge oncologist face today!
Wednesday, November 28, 2012
PARP Inhibitors
PARP
Day 2 went very well in Houston
made it on time
in the meantime received positive news from El Paso
can apply for faculty time in clinic at University Medical Center
will be an honor if it gets through'
willing to cover at another Hospital over coming holidays to broaden my share of patients
while veterans physicians take it easy...will use any opportunity to shine.
Now Back to PARP inhibitor, (Poly ADP Ribose Polymerase), they are powerful drugs which follow our first law, they break DNA or cause failure to repair DNA mistakes. Therefore cause automatic activation of intact P53 to induce automatic cell division Arrest. In other words, they act like Cisplatin and therefore will have a role in Ovarian cancer and by inference, will have a role in basal cell like Breast cancer (or triple negative Breast cancer). Again, their limitation depend on preservation of P53 and all other molecules of that cascade. They will also be limited by how fast the cell makes its repair.
Remember the 2nd law is the break of Microtubules/Microfilaments that leads to direct Caspase release, more powerful law. This implies that a combination of PARP with Taxane (or Ixabepilone or Erubilin)will be the next non platinum combination of significance.
Following this logic, we predict an expanded role to Arsenic trioxyde. But fear of its use resides in its cardiac toxicity. But it acts like a Multikinase inhibitor because it interferes with so many cascades in the signal transduction. Its limitation could also be that it may not lend itself to combination therapy because of "assumed" risk to the host.
Day 2 went very well in Houston
made it on time
in the meantime received positive news from El Paso
can apply for faculty time in clinic at University Medical Center
will be an honor if it gets through'
willing to cover at another Hospital over coming holidays to broaden my share of patients
while veterans physicians take it easy...will use any opportunity to shine.
Now Back to PARP inhibitor, (Poly ADP Ribose Polymerase), they are powerful drugs which follow our first law, they break DNA or cause failure to repair DNA mistakes. Therefore cause automatic activation of intact P53 to induce automatic cell division Arrest. In other words, they act like Cisplatin and therefore will have a role in Ovarian cancer and by inference, will have a role in basal cell like Breast cancer (or triple negative Breast cancer). Again, their limitation depend on preservation of P53 and all other molecules of that cascade. They will also be limited by how fast the cell makes its repair.
Remember the 2nd law is the break of Microtubules/Microfilaments that leads to direct Caspase release, more powerful law. This implies that a combination of PARP with Taxane (or Ixabepilone or Erubilin)will be the next non platinum combination of significance.
Following this logic, we predict an expanded role to Arsenic trioxyde. But fear of its use resides in its cardiac toxicity. But it acts like a Multikinase inhibitor because it interferes with so many cascades in the signal transduction. Its limitation could also be that it may not lend itself to combination therapy because of "assumed" risk to the host.
Sunday, November 25, 2012
SEARCHING FOR A CANCER CURE
At CRBCM we believe that CPRIT is our necessary path to Victory over Cancer.
We also know we will not get its help this time around, not because we do not deserve the help but frankly because it is distracted. Science is an objective thing. It is a race. You have the right move, the right stuff, you win, no matter where you come from. It is the Olympics without steroids.
We at CRBCM have understood one thing, in the race for the cure, harnessing the force and laws of nature has an unparalleled advantage. Forcing a cell to die can be done by telling and convincing it to die. Or blasting it and crossing our fingers and hoping it will die. Chemotherapy did this mostly the second way but its success was partial. Chemotherapy only works when it manages to finally talk the language. Indeed, some chemotherapy manages to reach the syllables of the cellular language of death.
Sorting through the maze of messages, 2 powerful set of syllables come out:
1. That if it fails to repair broken DNA and therefore does not perform GENE REPAIR, this fact will automatically activate your P53 leading to an automatic stop of the cell into its cycle division. There is no loophole to this principle unless the P53 is abnormal. Knowing this is powerful. Now we understand why Cisplatin (and to some extent Gemcitabine) is a powerful drug because it disrupts the DNA structure. We also understand that cells with rapid repair of DNA, will brush it off, literally.
2.with further proof of principle, we believe that there is a second automatic message or syllables.
Destruction of Microfilaments (and therefore secondarily Microtubules in general) during cell division, leads to an automatic release of Caspase from the Mitochondria no matter what (and this is what includes the BCL-2 protection). It is in this law that resides the strength of Taxanes. Medication that works even in resistant diseases such as Melanoma where Abraxane has a role. Taxanes' limitations appear to be in the type of microtubules attacked. Medication that attacks Microfilament of the type involved in cell divison, where the Centromere is attached, appears to send a more determinant trigger to Caspase release. This is where our interest comes in the Anti-kinesin. We believe and predict that an effective anti-kinesin drug in combination with Taxane and Cisplatin/gemzar based combination, will harness best this law. They will prove to be effective in cure because they will be effective in both treatment and maintenance settings. This is also why the combination of Gemzar and Taxol has proven to be the strongest non platinum combination.
Following this principle, we believe now at CRBCM, that target therapy not following the laws of nature will have only 20-30% response rate, meaning effective in only the cells that lack loophole mechanisms. (this also means because of phenotype heterogeneity, 70-85% of cells have potentially intrinsic loophole to any signal transduction target stimulation or blockage).
Lets keep our eyes on the ball, do not invest in stuff they are throwing at you! More to come...
At CRBCM we believe that CPRIT is our necessary path to Victory over Cancer.
We also know we will not get its help this time around, not because we do not deserve the help but frankly because it is distracted. Science is an objective thing. It is a race. You have the right move, the right stuff, you win, no matter where you come from. It is the Olympics without steroids.
We at CRBCM have understood one thing, in the race for the cure, harnessing the force and laws of nature has an unparalleled advantage. Forcing a cell to die can be done by telling and convincing it to die. Or blasting it and crossing our fingers and hoping it will die. Chemotherapy did this mostly the second way but its success was partial. Chemotherapy only works when it manages to finally talk the language. Indeed, some chemotherapy manages to reach the syllables of the cellular language of death.
Sorting through the maze of messages, 2 powerful set of syllables come out:
1. That if it fails to repair broken DNA and therefore does not perform GENE REPAIR, this fact will automatically activate your P53 leading to an automatic stop of the cell into its cycle division. There is no loophole to this principle unless the P53 is abnormal. Knowing this is powerful. Now we understand why Cisplatin (and to some extent Gemcitabine) is a powerful drug because it disrupts the DNA structure. We also understand that cells with rapid repair of DNA, will brush it off, literally.
2.with further proof of principle, we believe that there is a second automatic message or syllables.
Destruction of Microfilaments (and therefore secondarily Microtubules in general) during cell division, leads to an automatic release of Caspase from the Mitochondria no matter what (and this is what includes the BCL-2 protection). It is in this law that resides the strength of Taxanes. Medication that works even in resistant diseases such as Melanoma where Abraxane has a role. Taxanes' limitations appear to be in the type of microtubules attacked. Medication that attacks Microfilament of the type involved in cell divison, where the Centromere is attached, appears to send a more determinant trigger to Caspase release. This is where our interest comes in the Anti-kinesin. We believe and predict that an effective anti-kinesin drug in combination with Taxane and Cisplatin/gemzar based combination, will harness best this law. They will prove to be effective in cure because they will be effective in both treatment and maintenance settings. This is also why the combination of Gemzar and Taxol has proven to be the strongest non platinum combination.
Following this principle, we believe now at CRBCM, that target therapy not following the laws of nature will have only 20-30% response rate, meaning effective in only the cells that lack loophole mechanisms. (this also means because of phenotype heterogeneity, 70-85% of cells have potentially intrinsic loophole to any signal transduction target stimulation or blockage).
Lets keep our eyes on the ball, do not invest in stuff they are throwing at you! More to come...
Labels:
abraxane,
anti-kinesin,
caspase,
cell division,
centromere,
cisplatin,
cprit,
crbcm,
cycle division,
gemcitabine,
gemzar,
gene repair,
microfilaments,
microtubules,
P53,
taxane,
taxol
Friday, November 2, 2012
The secret for Cure of cancer is located in the selective apoptosis, or cancer cell death
We know there are several ways that lead to cell death. The main 2 ways are through the Extrinsic pathway which uses Receptors located at the skin of the cell called cellular membrane (receptors such as TNF-R1 and FAS) and Intrinsic pathways that use internal proteins (i.e. Caspases) that may destroy or paralyze the breathing and energy producing organs of the cell called mitochondria. The challenge is to control these processes in the cell, know how to trigger them, and to do this only in the cancer cells without affecting the normal cells. We need to know how to tag cancer cells, give that tag to a killing molecule that can attach to the apoptosis receptor. This is just one way to be looking for a cure. The complexity and multitude of metabolic pathways presents a problem, but also opportunities to kill the cancer cell.We are in the wee hours of learning them.Target therapy is in its early hour.
When there is a mistake in the gene during replication, there is a repair mechanism. To allow that repair,
the cell needs to be slowed down in its life cycle. This slowing seems to be the main action of P53. If repair does not occur, P53 leads the cell to cell destruction/apoptosis. That's why most cancers remove or change the P53 to stay alive. Like most Molecules in the cell, the P53 has its own path to destruction. MDM2 seems to be that path to the loss of this so important P53. Scientists are looking at knocking down MDM2 to see if this may restore the P53 function in those conditions where the P53 is not fundamentally altered. We will follow this for you and give an update!
The Cure is achievable we know that for sure, we need just need to become better "cell mechanics"....stay tuned...
When there is a mistake in the gene during replication, there is a repair mechanism. To allow that repair,
the cell needs to be slowed down in its life cycle. This slowing seems to be the main action of P53. If repair does not occur, P53 leads the cell to cell destruction/apoptosis. That's why most cancers remove or change the P53 to stay alive. Like most Molecules in the cell, the P53 has its own path to destruction. MDM2 seems to be that path to the loss of this so important P53. Scientists are looking at knocking down MDM2 to see if this may restore the P53 function in those conditions where the P53 is not fundamentally altered. We will follow this for you and give an update!
The Cure is achievable we know that for sure, we need just need to become better "cell mechanics"....stay tuned...
Sunday, October 21, 2012
Clinical Hypothesis in research, prevention and Commercialization Hypothesis in cancer therapeutics
Following our first article of October 14th, we believe it is time to suggest a second hypothesis
in therapeutic research in Cancer. The early years of cancer treatment, the objective was to blast the cancer cells with chemotherapy that was in our arsenal. Most of the time this approach was able to kill the cells partially. The cancer cells quickly however learned to escape the blast, creating wonderful resistance mechanisms. As we progress in molecular biology, we are increasingly shying away from these blast approaches, leaning more and more in identifying metabolic pathways, and identifying targets in that pathway and aiming our gun and shoot it, and see what happens. This is called Target Therapy.
One pathway that we have learned a bit about is the P53 ( and down the line the pathway the Rb which lead to cell stopping in the cell cycle to allow genetic repair). This pathway is mostly triggered by an abnormality in the gene.
Today, we go back to the blast approach when we have no good Target therapy option. In fact we always try to add the target therapy to the blast chemotherapy to see if we could have the most from our money.
combination of Avastin (a target therapy) to chemotherapy is standard therapy in the United states for stage IV Colon cancer. We know that chemotherapy mostly affect our gene. This change in gene should trigger the activation of our P53 system to stop the cancer cell in its track for growth. The question now is should we give chemotherapy in patient who has an altered P53 system. What is the benefit the gene with chemotherapy, if the system that should be triggered to clean up is out.
Hypothesis:
Altered P53 pathway predict a failure of chemotherapy which has gene disturbance as main effect.
second hypothesis: preservation of status of the wild type P53 during chemotherapy may predict for a successful chemotherapy treatment (Cisplatin).
if it is true, commercialization is possible...
Don't be shy, give me your opinion!
in therapeutic research in Cancer. The early years of cancer treatment, the objective was to blast the cancer cells with chemotherapy that was in our arsenal. Most of the time this approach was able to kill the cells partially. The cancer cells quickly however learned to escape the blast, creating wonderful resistance mechanisms. As we progress in molecular biology, we are increasingly shying away from these blast approaches, leaning more and more in identifying metabolic pathways, and identifying targets in that pathway and aiming our gun and shoot it, and see what happens. This is called Target Therapy.
One pathway that we have learned a bit about is the P53 ( and down the line the pathway the Rb which lead to cell stopping in the cell cycle to allow genetic repair). This pathway is mostly triggered by an abnormality in the gene.
Today, we go back to the blast approach when we have no good Target therapy option. In fact we always try to add the target therapy to the blast chemotherapy to see if we could have the most from our money.
combination of Avastin (a target therapy) to chemotherapy is standard therapy in the United states for stage IV Colon cancer. We know that chemotherapy mostly affect our gene. This change in gene should trigger the activation of our P53 system to stop the cancer cell in its track for growth. The question now is should we give chemotherapy in patient who has an altered P53 system. What is the benefit the gene with chemotherapy, if the system that should be triggered to clean up is out.
Hypothesis:
Altered P53 pathway predict a failure of chemotherapy which has gene disturbance as main effect.
second hypothesis: preservation of status of the wild type P53 during chemotherapy may predict for a successful chemotherapy treatment (Cisplatin).
if it is true, commercialization is possible...
Don't be shy, give me your opinion!
Subscribe to:
Posts (Atom)