The reading about mechanisms of resistance of to Taxol calls for a new strategy for treatment of triple negative breast cancer; while it is true that PARP inhibitor should still be considered in BRCA positive cancers, adding AURORA inhibitors seems to offer logically the best opportunity to increase the activity of proposed first line drugs.
Indeed, triple negative breast cancer assumes that the receptors to conventional stimulants of the breast cancer cell are not functional or responsive. Therefore, increasing the role of a direct attack of either the nuclear material or the microfilament/microtubule. Taxol - Cisplatin combination achieves that! Adding Avastin and other receptor stimulators could be a riskier proposition if you assume a questionable sensitivity of receptor in general. Your best bet is an action on the Histones and further DNA destruction. The cell division is your focus here and this is re-emphasized by the importance of CDKs as described by MD Anderson researchers. As a matter of fact, the AURORA inhibitors by binding to Adenine and to the Histone appear to offer a potential and logical choice to recruit in first line to boost response rates! So, pending proof of concept, we support the idea of adding Aurora inhibitors to a Taxane-Cisplatin core combination. Some of the Aurora Kinase also target CDKs and JAK2. These will be my choice for new trials!
After the cancer has seen chemotherapy, endothelial cells have been altered, hypoxia has been triggered by closure of some of the blood vessel closure, the MTOR has been stimulated, we believe adding the MTOR makes more sense. This has been also suggested after failure of Avastin, These concepts have been publicized, It is time to move to clinical trial! (FOR THOSE WHO CAN, WE HAVE OUR HANDS TIED BY HUMAN HISTORY!)
A blog about research, awareness, prevention, treatment and survivorship of Breast Cancer and all cancers, including targeted scientific research and a grassroots approach to increase screening for cancer, especially in the low income and under-insured population of El Paso, Texas, with a view to expand this new health care model to many other 'minority' populations across the United States and beyond
Showing posts with label cisplatin. Show all posts
Showing posts with label cisplatin. Show all posts
Tuesday, April 30, 2013
Tuesday, April 2, 2013
Nomenclature of genes in Esophageal cancer (continued)
FEZ1 , fasciculation and Elongation protein Zeta,
a significant gene intervening in the motility of the Esophagus.
Alteration of this gene also increases cancer susceptibility to viral infection (HIV).
It interacts with NBR1, a gene that confers a certain refractoriness to this cancer
and supports the Idea that Cisplatin may be essential to treatment in this disease.
In fact, several neurological receptors are involved in Esophageal cancer
and may contribute to the disease's poor prognosis and epithelial morphology presentation.
RHBF2
--------
a significant gene intervening in the motility of the Esophagus.
Alteration of this gene also increases cancer susceptibility to viral infection (HIV).
It interacts with NBR1, a gene that confers a certain refractoriness to this cancer
and supports the Idea that Cisplatin may be essential to treatment in this disease.
In fact, several neurological receptors are involved in Esophageal cancer
and may contribute to the disease's poor prognosis and epithelial morphology presentation.
RHBF2
--------
Saturday, March 16, 2013
THE AURORA KINASES
ONCE AGAIN YOU SEE HOW THE CELL PLAYS, USING SIMPLE THINGS THAT GET COMPLICATED REALLY QUICKLY!
Given our current understanding of the way they are suppressed by normal activity of P53, the aurora Kinase inhibitors should be used in cancers where P53 is clearly dys-regulated, and probably in disease with positive Prostate Stem Cell Antigen. This open the door to Sarcomas (chondrosarcoma being the most cited) and Pancreatic cancers (as well as Bladder cancers).
GADD45, a P53 dependent protein that inhibits Cdc2/Cyclin B1 could therefore be the best predictor of Aurora activity.
Quantification of CDCA8/Borealin, BIRC5/survivin, and INCENP may provide additional information on AURORA KINASE ACTIVITY. Like the core Binding Factor, these 3 Molecules form the Chromosomal Passenger Complex (CPC) which interact with POGZ, EVI5, and JTB.
Niehrs at al further define the role of GADD45 as "Gadd45 recruits nucleotide and/or base excision repair factors to gene-specific loci and acts as an adapter between repair factors and chromatin, thereby creating a nexus between epigenetics and DNA repair." Therefore explaining how P53 induced arrest is followed by DNA repair through recruitment of GADD45. When the cell is trying to repair itself with increase in GADD45, of course it wont want to die, therefore over-expression of GADD45 decrease the c-JUN, protecting therefore from TNF induced apoptosis. GADD45 is not good theoretically when you use Cisplatin or radiation for that matter!
*POGZ explains Nuclear transposition of P53 effects as it impacts SP1, a transcription factor with inteaction of all major playors in the cell including E2F1, POU2F1. YOU TARGET SP1 WITH WITH AFERIN FOR EXAMPLE, IT IS IMPOSSIBLE TO COME UP EMPTY HANDED.
*EVI5
"Identification of Rab11 as a small GTPase binding protein for the Evi5 oncogene"
Protein JTB also known as the jumping translocation breakpoint protein or prostate androgen-regulated protein (PAR) is a protein that in humans is encoded by the JTB gene.[1][2]
The JTB family of proteins contains several jumping translocation breakpoint proteins or JTBs. Jumping translocation (JT) is an unbalanced translocation that comprises amplified chromosomal segments jumping to various telomeres. JTB has been found to fuse with the telomeric repeats of acceptor telomeres in a case of JT. Homo sapiens JTB (hJTB) encodes a transmembrane protein that is highly conserved among divergent eukaryotic species. JT results in a hJTB truncation, which potentially produces an hJTB product devoid of the transmembrane domain. hJTB is located in a gene-rich region at 1q21, called EDC (Epidermal Differentiation Complex).[1] JTB has also been implicated in prostatic carcinomas.[3]
KANOME ET AL SUGGESTED
"JTB-induced clustering of mitochondria around the nuclear periphery and swelling of each mitochondrion. In those mitochondria, membrane potential, as monitored with a JC-1 probe, was significantly reduced. Coinciding with these changes in mitochondria, JTB retarded the growth of the cells and conferred resistance to TGF- 1-induced
apoptosis. These activities were dependent on the N-terminal processing
and induced by wild-type JTB but not by a mutant resistant to cleavage.
These findings raised the possibility that aberration of JTB in
structure or expression induced neoplastic changes in cells through
dysfunction of mitochondria leading to deregulated cell growth and/or
death."
1-induced
apoptosis. These activities were dependent on the N-terminal processing
and induced by wild-type JTB but not by a mutant resistant to cleavage.
These findings raised the possibility that aberration of JTB in
structure or expression induced neoplastic changes in cells through
dysfunction of mitochondria leading to deregulated cell growth and/or
death."
==================================================================
ONCE AGAIN YOU SEE HOW THE CELL PLAYS, USING SIMPLE THINGS THAT GET COMPLICATED REALLY QUICK!
Given our current understanding of the way they are suppressed by normal activity of P53, the aurora Kinase inhibitors should be used in cancers where P53 is clearly dys-regulated, and probably in disease with positive Prostate Stem Cell Antigen. This open the door to Sarcomas (chondrosarcoma being the most cited) and Pancreatic cancers (as well as Bladder cancers).
GADD45, a P53 dependent protein that inhibits Cdc2/Cyclin B1 could therefore be the best predictor of Aurora activity.
Quantification of CDCA8/Borealin, BIRC5/survivin, and INCENP may provide additional information on AURORA KINASE ACTIVITY. Like the core Binding Factor, these 3 Molecules form the Chromosomal Passenger Complex (CPC) which interact with POGZ, EVI5, and JTB.
Niehrs at al further define the role of GADD45 as "Gadd45 recruits nucleotide and/or base excision repair factors to gene-specific loci and acts as an adapter between repair factors and chromatin, thereby creating a nexus between epigenetics and DNA repair." Therefore explaining how P53 induced arrest is followed by DNA repair through recruitment of GADD45. When the cell is trying to repair itself with increase in GADD45, of course it wont want to die, therefore over-expression of GADD45 decrease the c-JUN, protecting therefore from TNF induced apoptosis. GADD45 is not good theoretically when you use Cisplatin or radiation for that matter!
*POGZ explains Nuclear transposition of P53 effects as it impacts SP1, a transcription factor with inteaction of all major playors in the cell including E2F1, POU2F1. YOU TARGET SP1 WITH WITH AFERIN FOR EXAMPLE, IT IS IMPOSSIBLE TO COME UP EMPTY HANDED.
*EVI5
"Identification of Rab11 as a small GTPase binding protein for the Evi5 oncogene"
This article has been cited by other articles in PMC.
Abstract
The Evi5 oncogene has recently been shown to regulate the stability and accumulation of critical G1
cell cycle factors including Emi1, an inhibitor of the
anaphase-promoting complex/cyclosome, and cyclin A. Sequence analysis of
the amino terminus of Evi5 reveals a Tre-2, Bub2, Cdc16 domain, which
has been shown to be a binding partner and GTPase-activating protein
domain for the Rab family of small Ras-like GTPases. Here we describe
the identification of Evi5 as a candidate binding protein for Rab11, a
GTPase that regulates intracellular transport and has specific roles in
endosome recycling and cytokinesis. By yeast two-hybrid analysis,
immunoprecipitation, and Biacore analysis, we demonstrate that Evi5
binds Rab11a and Rab11b in a GTP-dependent manner. However, Evi5
displays no activation of Rab11 GTPase activity in vitro. Evi5 colocalizes with Rab11 in vivo,
and overexpression of Rab11 perturbs the localization of Evi5,
redistributing it into Rab11-positive recycling endosomes.
Interestingly, in vitro binding studies show that Rab11
effector proteins including FIP3 compete with Evi5 for binding to Rab11,
suggesting a partitioning between Rab11–Evi5 and Rab11 effector
complexes. Indeed, ablation of Evi5 by RNA interference causes a
mislocalization of FIP3 at the abscission site during cytokinesis. These
data demonstrate that Evi5 is a Rab11 binding protein and that Evi5 may
cooperate with Rab11 to coordinate vesicular trafficking, cytokinesis,
and cell cycle control independent of GTPase-activating protein
function.
Keywords: cytokinesis, GTPase-activating protein, recycling endosome".
*JTB
JTB (gene)
From Wikipedia, the free encyclopedia
Jump to: navigation, search
| Jumping translocation breakpoint | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
|
|||||||||||
| Identifiers | |||||||||||
| Symbols | JTB; HJTB; HSPC222; PAR; hJT | ||||||||||
| External IDs | OMIM: 604671 MGI: 1346082 HomoloGene: 4870 GeneCards: JTB Gene | ||||||||||
|
|||||||||||
| RNA expression pattern | |||||||||||
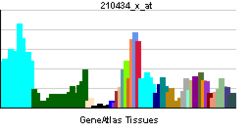 |
|||||||||||
 |
|||||||||||
| More reference expression data | |||||||||||
| Orthologs | |||||||||||
| Species | Human | Mouse | |||||||||
| Entrez | 10899 | 23922 | |||||||||
| Ensembl | ENSG00000143543 | ENSMUSG00000027937 | |||||||||
| UniProt | O76095 | O88824 | |||||||||
| RefSeq (mRNA) | NM_006694 | NM_206924 | |||||||||
| RefSeq (protein) | NP_006685 | NP_996807 | |||||||||
| Location (UCSC) | Chr 1: 153.95 – 153.95 Mb |
Chr 3: 90.23 – 90.24 Mb |
|||||||||
| PubMed search | [1] | [2] | |||||||||
| Jumping translocation breakpoint protein (JTB) | |||
|---|---|---|---|
| Identifiers | |||
| Symbol | JTB | ||
| Pfam | PF05439 | ||
| InterPro | IPR008657 | ||
|
|||
The JTB family of proteins contains several jumping translocation breakpoint proteins or JTBs. Jumping translocation (JT) is an unbalanced translocation that comprises amplified chromosomal segments jumping to various telomeres. JTB has been found to fuse with the telomeric repeats of acceptor telomeres in a case of JT. Homo sapiens JTB (hJTB) encodes a transmembrane protein that is highly conserved among divergent eukaryotic species. JT results in a hJTB truncation, which potentially produces an hJTB product devoid of the transmembrane domain. hJTB is located in a gene-rich region at 1q21, called EDC (Epidermal Differentiation Complex).[1] JTB has also been implicated in prostatic carcinomas.[3]
KANOME ET AL SUGGESTED
"JTB-induced clustering of mitochondria around the nuclear periphery and swelling of each mitochondrion. In those mitochondria, membrane potential, as monitored with a JC-1 probe, was significantly reduced. Coinciding with these changes in mitochondria, JTB retarded the growth of the cells and conferred resistance to TGF-
 1-induced
apoptosis. These activities were dependent on the N-terminal processing
and induced by wild-type JTB but not by a mutant resistant to cleavage.
These findings raised the possibility that aberration of JTB in
structure or expression induced neoplastic changes in cells through
dysfunction of mitochondria leading to deregulated cell growth and/or
death."
1-induced
apoptosis. These activities were dependent on the N-terminal processing
and induced by wild-type JTB but not by a mutant resistant to cleavage.
These findings raised the possibility that aberration of JTB in
structure or expression induced neoplastic changes in cells through
dysfunction of mitochondria leading to deregulated cell growth and/or
death."==================================================================
ONCE AGAIN YOU SEE HOW THE CELL PLAYS, USING SIMPLE THINGS THAT GET COMPLICATED REALLY QUICK!
Labels:
aurora kinases,
bladder cancer,
borealin,
CDC2,
CDCA8,
chondrosarcoma,
cisplatin,
crbcm,
Cyclin B1,
dysregulation,
kinase inhibitors,
P53,
pancreatic cancer,
prostate stem cell antigen,
sarcoma
Saturday, March 9, 2013
TODAY'S CONFERENCE NEWS!
One thing is for sure: current clinical practice of Oncology is miles away from the cutting edge science advancing before it and there is a reason to this fact, only what is clearly established and approved by national institutions reaches the practicing Oncologist. And clearly, it is important that speakers during Oncology conferences reinvent themselves deep enough to understand the flow of information coming through. It is easy to tell who knows fully and who is trying to keep up among speakers. Navigating the world of research while keeping up with clinical studies is the challenge our speakers face.
1. In lung cancer
-------------------
*In Adenocarcinoma: Pemetrex +Cisplatin based treatment is still King prior to gene Mutation determination, in Metastatic setting and first line
*But when EGFR and positive is known, Erlotinib came on top! And when progression occurs,
continuing ERLOTINIB, but adding a chemotherapy doublet won!
*Despite great achievements by Target therapy in lung cancer, most of the time it is hard to prove survival benefits because most studies allow cross-over of those failing the chemotherapy-alone arm.
*Afatinib was superior to Cisplatin-Pemetrex in those with Del 19/L858R (EGFR mutation positive)
with Progression free survival 13.6 months Vs 6.9 months in metastatic setting.
*Increasingly, re-biopsy at recurrence is occurring to reassess the status of common Mutations.
It has noted that tumors which were EGFR positive, once they become resistant, they adopt small cell features and respond to Small cell regimens.
* When using a EGFR, continue the drug beyond resistance because in a limited MSKCC series, up to 25% of cancers experience a "FLARE" when TKI (Tyrosine Kinase Inhibitors) were discontinued. So, while considering options for 2nd line therapy, do not stop TKI.
*Currently tested Mutations:
EGFR, EML4-ALK fusion, MET amplification by FISH (not so much by IHC), ROS-1, PIK3CA (sometime FGFR1)
*"PROXIMITY" TO ROS1 WITH INSULIN RECEPTOR discussed
*IF EGFR positive, rarely you will find KRAS (exclusivity rule discussed)
*in lung cancer :
you find ROS1 in 1.5% of cases,
ALK + in 5% of cases
RET + in 2% of cases
EGFR + in 18% of cases
HER-2 in 2 % of cases
*Acinar Morphology a cue for ALK positive? and CRIZOTINIB is the answer!
*Now comes OR HAS ARRIVED THE PRACTICE OF "MULTIPLEX TESTING" FOR IDENTIFICATION OF SPECIFIC MUTATIONS.
*Of note: the study showing Taxotere equivalent to Gefitinib in lung cancer cases unscreened for EGFR mutation at onset of trial are challenging the notion of Early EGFR identification!
NEW GANETESPID (+TAXOTERE), THIS IS AN INHIBITOR OF HSP90, A CHAPERONE MOLECULE AND PD-L1 BMS936558
WITH THIS FRAME OF INFORMATION - GO TO WORK!
NEXT: METASTATIC MELANOMA
1. In lung cancer
-------------------
*In Adenocarcinoma: Pemetrex +Cisplatin based treatment is still King prior to gene Mutation determination, in Metastatic setting and first line
*But when EGFR and positive is known, Erlotinib came on top! And when progression occurs,
continuing ERLOTINIB, but adding a chemotherapy doublet won!
*Despite great achievements by Target therapy in lung cancer, most of the time it is hard to prove survival benefits because most studies allow cross-over of those failing the chemotherapy-alone arm.
*Afatinib was superior to Cisplatin-Pemetrex in those with Del 19/L858R (EGFR mutation positive)
with Progression free survival 13.6 months Vs 6.9 months in metastatic setting.
*Increasingly, re-biopsy at recurrence is occurring to reassess the status of common Mutations.
It has noted that tumors which were EGFR positive, once they become resistant, they adopt small cell features and respond to Small cell regimens.
* When using a EGFR, continue the drug beyond resistance because in a limited MSKCC series, up to 25% of cancers experience a "FLARE" when TKI (Tyrosine Kinase Inhibitors) were discontinued. So, while considering options for 2nd line therapy, do not stop TKI.
*Currently tested Mutations:
EGFR, EML4-ALK fusion, MET amplification by FISH (not so much by IHC), ROS-1, PIK3CA (sometime FGFR1)
*"PROXIMITY" TO ROS1 WITH INSULIN RECEPTOR discussed
*IF EGFR positive, rarely you will find KRAS (exclusivity rule discussed)
*in lung cancer :
you find ROS1 in 1.5% of cases,
ALK + in 5% of cases
RET + in 2% of cases
EGFR + in 18% of cases
HER-2 in 2 % of cases
*Acinar Morphology a cue for ALK positive? and CRIZOTINIB is the answer!
*Now comes OR HAS ARRIVED THE PRACTICE OF "MULTIPLEX TESTING" FOR IDENTIFICATION OF SPECIFIC MUTATIONS.
*Of note: the study showing Taxotere equivalent to Gefitinib in lung cancer cases unscreened for EGFR mutation at onset of trial are challenging the notion of Early EGFR identification!
NEW GANETESPID (+TAXOTERE), THIS IS AN INHIBITOR OF HSP90, A CHAPERONE MOLECULE AND PD-L1 BMS936558
WITH THIS FRAME OF INFORMATION - GO TO WORK!
NEXT: METASTATIC MELANOMA
Wednesday, February 27, 2013
PREVENTABLE CANCER DEATH, AND YOU CAN'T DO A THING! AND THIS IS TEXAS/ USA!
HOW DO YOU LOOK AT A MAN 2 YEARS BEFORE HIS PREVENTABLE CANCER DEATH, AND YOU CAN'T DO A THING! AND THIS IS TEXAS/ USA!
Just got off the phone with a wife of a man with stage IIIB Penile cancer. Their largest problem is not the cancer, but the lack of insurance and lack of money. He needs Cisplatin, a drug older than myself, but can't afford it. He has positive inguinal node but can't afford a consultation with the radiation therapy DR. What to do? As an Oncologist I am offering my service, but this is not going to save the man.
It is a time like this that challenges your soul, you just want to run from this misery of mind and hide!
It is a time like this that universal Insurance makes complete sense, but it will come too late for this one man!
If you can help, call our clinic 915-307- 3354! And it is not the only case, I also have this 38 year old woman with unresectable Angiosarcomas in the liver.... same story....call if you can help!
Just got off the phone with a wife of a man with stage IIIB Penile cancer. Their largest problem is not the cancer, but the lack of insurance and lack of money. He needs Cisplatin, a drug older than myself, but can't afford it. He has positive inguinal node but can't afford a consultation with the radiation therapy DR. What to do? As an Oncologist I am offering my service, but this is not going to save the man.
It is a time like this that challenges your soul, you just want to run from this misery of mind and hide!
It is a time like this that universal Insurance makes complete sense, but it will come too late for this one man!
If you can help, call our clinic 915-307- 3354! And it is not the only case, I also have this 38 year old woman with unresectable Angiosarcomas in the liver.... same story....call if you can help!
Thursday, February 14, 2013
RANDOM NEWS with updates for Letrozole
*BIG 1-98 showed that LETROZOLE was more effective in post-menopausal patient with any histology of breast cancer that is ER positive and Her-2 Negative, with the effect being greater in lobular type of Carcinoma. And in Luminal B versus Luminal A.
* In HER-2 positive, one year Vs 2 Years.
"2 year long treatment not recommended",
finding of the HERA trial remains the standard of care.
In the study of 6 months Vs 12 months of Herceptin, there was a trend toward better results with 12 months also statistically no difference was detected.
*In Early Breast cancer, High Baseline of Vitamin D level was a predictor of 3 things:
1. better prognosis
2. low risk bone relapse
3. better outcome with use of Zometa.
recommendation is to measure Vit D at diagnosis and to replenish it!
*In triple negative breast cancer, the disease would be amenable to new type combinations of medications such as
A/ Cisplatin /PARP (olaprib) and Vandetanib (EGFR/VEGF).
B/ Cisplatin/PARP inhibitor and Vorinostat (Histone deacetylase inhibitor)
C/ Androgen Inhibitors and MTOR
*PD 0332991, an oral Cyclin dependent Kinase (CDK 4/6) inhibitor added to Letrozole increased the progression free from 7.5 months to 26.1 months. This is an impressive performance if confirmed.
*PIM-1 may be a surrogate of c-MYC amplification, and is being targeted.
* Routine Breast MRI still not recommended
*32mg IV Ondansetron can cause Arrhythmia and has been withdrawn.
* In HER-2 positive, one year Vs 2 Years.
"2 year long treatment not recommended",
finding of the HERA trial remains the standard of care.
In the study of 6 months Vs 12 months of Herceptin, there was a trend toward better results with 12 months also statistically no difference was detected.
*In Early Breast cancer, High Baseline of Vitamin D level was a predictor of 3 things:
1. better prognosis
2. low risk bone relapse
3. better outcome with use of Zometa.
recommendation is to measure Vit D at diagnosis and to replenish it!
*In triple negative breast cancer, the disease would be amenable to new type combinations of medications such as
A/ Cisplatin /PARP (olaprib) and Vandetanib (EGFR/VEGF).
B/ Cisplatin/PARP inhibitor and Vorinostat (Histone deacetylase inhibitor)
C/ Androgen Inhibitors and MTOR
*PD 0332991, an oral Cyclin dependent Kinase (CDK 4/6) inhibitor added to Letrozole increased the progression free from 7.5 months to 26.1 months. This is an impressive performance if confirmed.
*PIM-1 may be a surrogate of c-MYC amplification, and is being targeted.
* Routine Breast MRI still not recommended
*32mg IV Ondansetron can cause Arrhythmia and has been withdrawn.
Thursday, January 10, 2013
TRIPLE NEGATIVE BREAST CANCER, A MELTING POT
The news that the Genome of triple negative breast cancer is similar to ovarian cancer has been good as a starting point. But that is as far as it goes! Researcher are now scrambling trying to see how to best use this information and there is not one good direction. In fact if anything, it may have complicated the landscape.
The controversy is compounded by the news that there is not simply a single type of Triple Negative Breast cancer. This added to the fact that there is not just one type of Ovarian cancer. So which one is the best approach? And there are no known good suggestions, because of a lack of comprehensive database for cancer types. Our cancer knowledge is disconnected. Someone knows more about this. Someone else knows about that. There are Gaps in the knowledge which prevents us from moving forward.
Some of the facts and knowledge:
1. That the Genome is similar to Ovarian Cancer.
2. That Taxane-Cisplatin works in Ovarian Cancer
3. That PARP may have a role
4. That (low) MEKK1 expression is linked to tumor Response to Cisplatin.
5. That BRAC may impart a poor prognosis to the tumor
6. That Downregulation of STAT1 may play a role in the Oncogenesis of Triple Negative Breast cancer.
7. The almost total lack of Role of P53 alteration
8. Limited role of Kras Mutation
etc.
There are Major Questions of therapeutic importance:
1.Are these cancers MUCINOUS? Is there presence of MUC family members?
If these tumors are mucinous, this is another bad news. Mucin presence shields against detection by the innate immune system and favors cancer dissemination to go undetected. Mucin contains molecules that interfere with Glycocalyx, blunting their ability to expose cancer cells to the immune system, and also contain molecules full of Sulfhydryl expressing molecules which have profound interaction with electron based reactions at the membrane and Intracellularly. These activities are generally protective for the cancer cell.
The Mucinous presence can also be supported by the presence of Galectin 4 (LGALS4) 19q13.3 (Heterozygosity site). Positive TFF1 of the trefoil factor family which is an Estrogen regulated molecule that could potentially predict some response to hormone manipulation even in triple negative setting.
Amplification of CDX which modulate proliferation, cell adhesion and Apoptosis. The fact is this CDX could be a driver phenomena as this cancer is known for its ability to have a steady progression.
OTHER Molecules of Importance CDH17, Tetraspanin, MSF1R, E-Cadherin and the Kruppel like factor.
2. These tumors seems to have a survival that is epic, raising the issue of expression of survival pathways MEK, MAP Kinases and C-jun
3. What differentiates Endometrioid Vs other ovarian cancers will play a role in this disease
4. What is the role of target therapy, important in Ovarian cancer, as it relates to Triple negative breast cancer?
We are only just scratching the surface of this problem,
Time to put the puzzle together!
The news that the Genome of triple negative breast cancer is similar to ovarian cancer has been good as a starting point. But that is as far as it goes! Researcher are now scrambling trying to see how to best use this information and there is not one good direction. In fact if anything, it may have complicated the landscape.
The controversy is compounded by the news that there is not simply a single type of Triple Negative Breast cancer. This added to the fact that there is not just one type of Ovarian cancer. So which one is the best approach? And there are no known good suggestions, because of a lack of comprehensive database for cancer types. Our cancer knowledge is disconnected. Someone knows more about this. Someone else knows about that. There are Gaps in the knowledge which prevents us from moving forward.
Some of the facts and knowledge:
1. That the Genome is similar to Ovarian Cancer.
2. That Taxane-Cisplatin works in Ovarian Cancer
3. That PARP may have a role
4. That (low) MEKK1 expression is linked to tumor Response to Cisplatin.
5. That BRAC may impart a poor prognosis to the tumor
6. That Downregulation of STAT1 may play a role in the Oncogenesis of Triple Negative Breast cancer.
7. The almost total lack of Role of P53 alteration
8. Limited role of Kras Mutation
etc.
There are Major Questions of therapeutic importance:
1.Are these cancers MUCINOUS? Is there presence of MUC family members?
If these tumors are mucinous, this is another bad news. Mucin presence shields against detection by the innate immune system and favors cancer dissemination to go undetected. Mucin contains molecules that interfere with Glycocalyx, blunting their ability to expose cancer cells to the immune system, and also contain molecules full of Sulfhydryl expressing molecules which have profound interaction with electron based reactions at the membrane and Intracellularly. These activities are generally protective for the cancer cell.
The Mucinous presence can also be supported by the presence of Galectin 4 (LGALS4) 19q13.3 (Heterozygosity site). Positive TFF1 of the trefoil factor family which is an Estrogen regulated molecule that could potentially predict some response to hormone manipulation even in triple negative setting.
Amplification of CDX which modulate proliferation, cell adhesion and Apoptosis. The fact is this CDX could be a driver phenomena as this cancer is known for its ability to have a steady progression.
OTHER Molecules of Importance CDH17, Tetraspanin, MSF1R, E-Cadherin and the Kruppel like factor.
2. These tumors seems to have a survival that is epic, raising the issue of expression of survival pathways MEK, MAP Kinases and C-jun
3. What differentiates Endometrioid Vs other ovarian cancers will play a role in this disease
4. What is the role of target therapy, important in Ovarian cancer, as it relates to Triple negative breast cancer?
We are only just scratching the surface of this problem,
Time to put the puzzle together!
Wednesday, November 28, 2012
PARP Inhibitors
PARP
Day 2 went very well in Houston
made it on time
in the meantime received positive news from El Paso
can apply for faculty time in clinic at University Medical Center
will be an honor if it gets through'
willing to cover at another Hospital over coming holidays to broaden my share of patients
while veterans physicians take it easy...will use any opportunity to shine.
Now Back to PARP inhibitor, (Poly ADP Ribose Polymerase), they are powerful drugs which follow our first law, they break DNA or cause failure to repair DNA mistakes. Therefore cause automatic activation of intact P53 to induce automatic cell division Arrest. In other words, they act like Cisplatin and therefore will have a role in Ovarian cancer and by inference, will have a role in basal cell like Breast cancer (or triple negative Breast cancer). Again, their limitation depend on preservation of P53 and all other molecules of that cascade. They will also be limited by how fast the cell makes its repair.
Remember the 2nd law is the break of Microtubules/Microfilaments that leads to direct Caspase release, more powerful law. This implies that a combination of PARP with Taxane (or Ixabepilone or Erubilin)will be the next non platinum combination of significance.
Following this logic, we predict an expanded role to Arsenic trioxyde. But fear of its use resides in its cardiac toxicity. But it acts like a Multikinase inhibitor because it interferes with so many cascades in the signal transduction. Its limitation could also be that it may not lend itself to combination therapy because of "assumed" risk to the host.
Day 2 went very well in Houston
made it on time
in the meantime received positive news from El Paso
can apply for faculty time in clinic at University Medical Center
will be an honor if it gets through'
willing to cover at another Hospital over coming holidays to broaden my share of patients
while veterans physicians take it easy...will use any opportunity to shine.
Now Back to PARP inhibitor, (Poly ADP Ribose Polymerase), they are powerful drugs which follow our first law, they break DNA or cause failure to repair DNA mistakes. Therefore cause automatic activation of intact P53 to induce automatic cell division Arrest. In other words, they act like Cisplatin and therefore will have a role in Ovarian cancer and by inference, will have a role in basal cell like Breast cancer (or triple negative Breast cancer). Again, their limitation depend on preservation of P53 and all other molecules of that cascade. They will also be limited by how fast the cell makes its repair.
Remember the 2nd law is the break of Microtubules/Microfilaments that leads to direct Caspase release, more powerful law. This implies that a combination of PARP with Taxane (or Ixabepilone or Erubilin)will be the next non platinum combination of significance.
Following this logic, we predict an expanded role to Arsenic trioxyde. But fear of its use resides in its cardiac toxicity. But it acts like a Multikinase inhibitor because it interferes with so many cascades in the signal transduction. Its limitation could also be that it may not lend itself to combination therapy because of "assumed" risk to the host.
Sunday, November 25, 2012
SEARCHING FOR A CANCER CURE
At CRBCM we believe that CPRIT is our necessary path to Victory over Cancer.
We also know we will not get its help this time around, not because we do not deserve the help but frankly because it is distracted. Science is an objective thing. It is a race. You have the right move, the right stuff, you win, no matter where you come from. It is the Olympics without steroids.
We at CRBCM have understood one thing, in the race for the cure, harnessing the force and laws of nature has an unparalleled advantage. Forcing a cell to die can be done by telling and convincing it to die. Or blasting it and crossing our fingers and hoping it will die. Chemotherapy did this mostly the second way but its success was partial. Chemotherapy only works when it manages to finally talk the language. Indeed, some chemotherapy manages to reach the syllables of the cellular language of death.
Sorting through the maze of messages, 2 powerful set of syllables come out:
1. That if it fails to repair broken DNA and therefore does not perform GENE REPAIR, this fact will automatically activate your P53 leading to an automatic stop of the cell into its cycle division. There is no loophole to this principle unless the P53 is abnormal. Knowing this is powerful. Now we understand why Cisplatin (and to some extent Gemcitabine) is a powerful drug because it disrupts the DNA structure. We also understand that cells with rapid repair of DNA, will brush it off, literally.
2.with further proof of principle, we believe that there is a second automatic message or syllables.
Destruction of Microfilaments (and therefore secondarily Microtubules in general) during cell division, leads to an automatic release of Caspase from the Mitochondria no matter what (and this is what includes the BCL-2 protection). It is in this law that resides the strength of Taxanes. Medication that works even in resistant diseases such as Melanoma where Abraxane has a role. Taxanes' limitations appear to be in the type of microtubules attacked. Medication that attacks Microfilament of the type involved in cell divison, where the Centromere is attached, appears to send a more determinant trigger to Caspase release. This is where our interest comes in the Anti-kinesin. We believe and predict that an effective anti-kinesin drug in combination with Taxane and Cisplatin/gemzar based combination, will harness best this law. They will prove to be effective in cure because they will be effective in both treatment and maintenance settings. This is also why the combination of Gemzar and Taxol has proven to be the strongest non platinum combination.
Following this principle, we believe now at CRBCM, that target therapy not following the laws of nature will have only 20-30% response rate, meaning effective in only the cells that lack loophole mechanisms. (this also means because of phenotype heterogeneity, 70-85% of cells have potentially intrinsic loophole to any signal transduction target stimulation or blockage).
Lets keep our eyes on the ball, do not invest in stuff they are throwing at you! More to come...
At CRBCM we believe that CPRIT is our necessary path to Victory over Cancer.
We also know we will not get its help this time around, not because we do not deserve the help but frankly because it is distracted. Science is an objective thing. It is a race. You have the right move, the right stuff, you win, no matter where you come from. It is the Olympics without steroids.
We at CRBCM have understood one thing, in the race for the cure, harnessing the force and laws of nature has an unparalleled advantage. Forcing a cell to die can be done by telling and convincing it to die. Or blasting it and crossing our fingers and hoping it will die. Chemotherapy did this mostly the second way but its success was partial. Chemotherapy only works when it manages to finally talk the language. Indeed, some chemotherapy manages to reach the syllables of the cellular language of death.
Sorting through the maze of messages, 2 powerful set of syllables come out:
1. That if it fails to repair broken DNA and therefore does not perform GENE REPAIR, this fact will automatically activate your P53 leading to an automatic stop of the cell into its cycle division. There is no loophole to this principle unless the P53 is abnormal. Knowing this is powerful. Now we understand why Cisplatin (and to some extent Gemcitabine) is a powerful drug because it disrupts the DNA structure. We also understand that cells with rapid repair of DNA, will brush it off, literally.
2.with further proof of principle, we believe that there is a second automatic message or syllables.
Destruction of Microfilaments (and therefore secondarily Microtubules in general) during cell division, leads to an automatic release of Caspase from the Mitochondria no matter what (and this is what includes the BCL-2 protection). It is in this law that resides the strength of Taxanes. Medication that works even in resistant diseases such as Melanoma where Abraxane has a role. Taxanes' limitations appear to be in the type of microtubules attacked. Medication that attacks Microfilament of the type involved in cell divison, where the Centromere is attached, appears to send a more determinant trigger to Caspase release. This is where our interest comes in the Anti-kinesin. We believe and predict that an effective anti-kinesin drug in combination with Taxane and Cisplatin/gemzar based combination, will harness best this law. They will prove to be effective in cure because they will be effective in both treatment and maintenance settings. This is also why the combination of Gemzar and Taxol has proven to be the strongest non platinum combination.
Following this principle, we believe now at CRBCM, that target therapy not following the laws of nature will have only 20-30% response rate, meaning effective in only the cells that lack loophole mechanisms. (this also means because of phenotype heterogeneity, 70-85% of cells have potentially intrinsic loophole to any signal transduction target stimulation or blockage).
Lets keep our eyes on the ball, do not invest in stuff they are throwing at you! More to come...
Labels:
abraxane,
anti-kinesin,
caspase,
cell division,
centromere,
cisplatin,
cprit,
crbcm,
cycle division,
gemcitabine,
gemzar,
gene repair,
microfilaments,
microtubules,
P53,
taxane,
taxol
Sunday, October 21, 2012
Clinical Hypothesis in research, prevention and Commercialization Hypothesis in cancer therapeutics
Following our first article of October 14th, we believe it is time to suggest a second hypothesis
in therapeutic research in Cancer. The early years of cancer treatment, the objective was to blast the cancer cells with chemotherapy that was in our arsenal. Most of the time this approach was able to kill the cells partially. The cancer cells quickly however learned to escape the blast, creating wonderful resistance mechanisms. As we progress in molecular biology, we are increasingly shying away from these blast approaches, leaning more and more in identifying metabolic pathways, and identifying targets in that pathway and aiming our gun and shoot it, and see what happens. This is called Target Therapy.
One pathway that we have learned a bit about is the P53 ( and down the line the pathway the Rb which lead to cell stopping in the cell cycle to allow genetic repair). This pathway is mostly triggered by an abnormality in the gene.
Today, we go back to the blast approach when we have no good Target therapy option. In fact we always try to add the target therapy to the blast chemotherapy to see if we could have the most from our money.
combination of Avastin (a target therapy) to chemotherapy is standard therapy in the United states for stage IV Colon cancer. We know that chemotherapy mostly affect our gene. This change in gene should trigger the activation of our P53 system to stop the cancer cell in its track for growth. The question now is should we give chemotherapy in patient who has an altered P53 system. What is the benefit the gene with chemotherapy, if the system that should be triggered to clean up is out.
Hypothesis:
Altered P53 pathway predict a failure of chemotherapy which has gene disturbance as main effect.
second hypothesis: preservation of status of the wild type P53 during chemotherapy may predict for a successful chemotherapy treatment (Cisplatin).
if it is true, commercialization is possible...
Don't be shy, give me your opinion!
in therapeutic research in Cancer. The early years of cancer treatment, the objective was to blast the cancer cells with chemotherapy that was in our arsenal. Most of the time this approach was able to kill the cells partially. The cancer cells quickly however learned to escape the blast, creating wonderful resistance mechanisms. As we progress in molecular biology, we are increasingly shying away from these blast approaches, leaning more and more in identifying metabolic pathways, and identifying targets in that pathway and aiming our gun and shoot it, and see what happens. This is called Target Therapy.
One pathway that we have learned a bit about is the P53 ( and down the line the pathway the Rb which lead to cell stopping in the cell cycle to allow genetic repair). This pathway is mostly triggered by an abnormality in the gene.
Today, we go back to the blast approach when we have no good Target therapy option. In fact we always try to add the target therapy to the blast chemotherapy to see if we could have the most from our money.
combination of Avastin (a target therapy) to chemotherapy is standard therapy in the United states for stage IV Colon cancer. We know that chemotherapy mostly affect our gene. This change in gene should trigger the activation of our P53 system to stop the cancer cell in its track for growth. The question now is should we give chemotherapy in patient who has an altered P53 system. What is the benefit the gene with chemotherapy, if the system that should be triggered to clean up is out.
Hypothesis:
Altered P53 pathway predict a failure of chemotherapy which has gene disturbance as main effect.
second hypothesis: preservation of status of the wild type P53 during chemotherapy may predict for a successful chemotherapy treatment (Cisplatin).
if it is true, commercialization is possible...
Don't be shy, give me your opinion!
Subscribe to:
Comments (Atom)